Health Financing
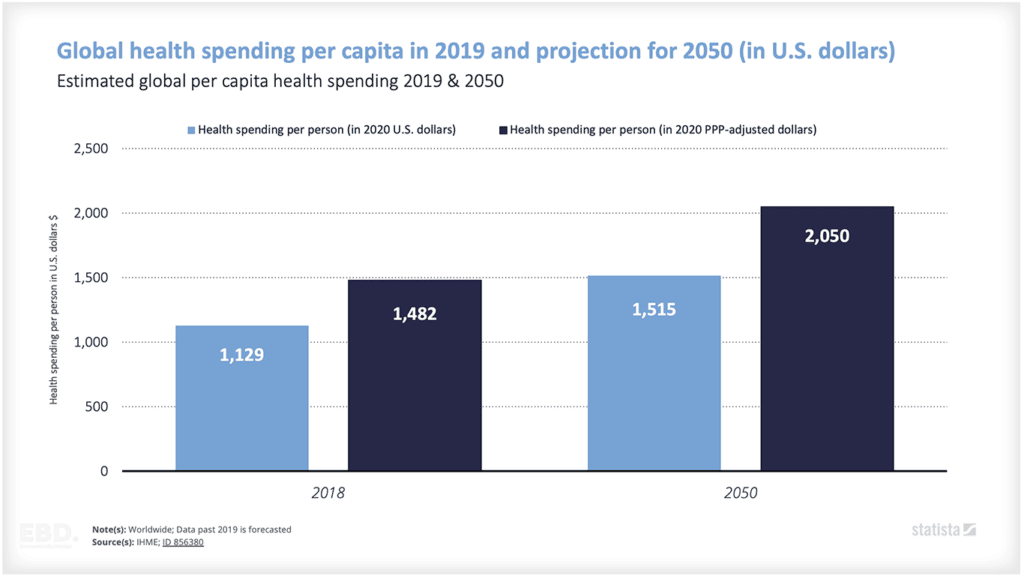
Health financing is a critical enabler of Universal Health Coverage (UHC). It ensures that people can access the universal coverage for health services they need without suffering financial hardship.
There are many different ways to flow funds through the health care system, but all systems have four basic elements:
Financing & Revenue Sources
This is when funds are gathered from people to pay for health care needs. This can be done at scale through government contributions, taxes, social insurance contributions, private insurance contributions, or philanthropic contributions. It also includes out-of-pocket payments by individuals paying directly for treatment when it is needed.
Risk Pooling
Funds gathered at scale can be pooled together in a way that allows them to be used more efficiently and effectively. This means that the risks of needing healthcare are shared among a larger group of people, which helps to keep costs down. Pooling can be done through a single fund for a whole health system, regional funds for sub-national systems, or multiple funds for specific population groups.
Strategic Purchasing
Pooled funds are used to purchase health care services for a group. This can be done directly by the government or through private insurers. It includes making contracts with providers, setting prices, and ensuring that quality standards are met.
Provider Payment Models
Providers (such as hospitals and doctors) need to be paid for the health care services they provide. This can be done through a variety of models, capitation, block funding, line-item funding, fee-for-service, case-based payments, or a mix of some or all. It can include incentives to improve performance or conditional on achieving pre-agreed outcomes.
The focus of this economics lens is on risk pooling or pooling funds.
Risk Pooling or Pooling Funds
The cost of providing healthcare services to an individual can be very high and very uncertain. Not everyone can afford to pay for their healthcare or even plan for the likely costs they may face over their lifetime.
It is very difficult for individuals to predict their health risks and the potential costs of health risks over their lifetime. Risks tend to increase at various stages of life (e.g. birth and early childhood, women giving birth, ageing) and as a result of harmful behaviours (e.g. smoking, excessive consumption of alcohol, poor levels of physical activity). Just to add a layer of complexity, variation in risk is largely determined by the wider social determinants of health (such as employment, housing, and environment).
For these reasons, individuals need to have access to a system that allows them to share the risk of suffering financial hardship as a result of ill health. By pooling funds, the risks of high healthcare costs arising from ill health are shared across a large number of people.
The WHO defines the purpose of risk-pooling as being “to spread financial risk across the population so that no individual carries the full burden of paying for health care”.
What Are The Different Classes of Risk Pooling?
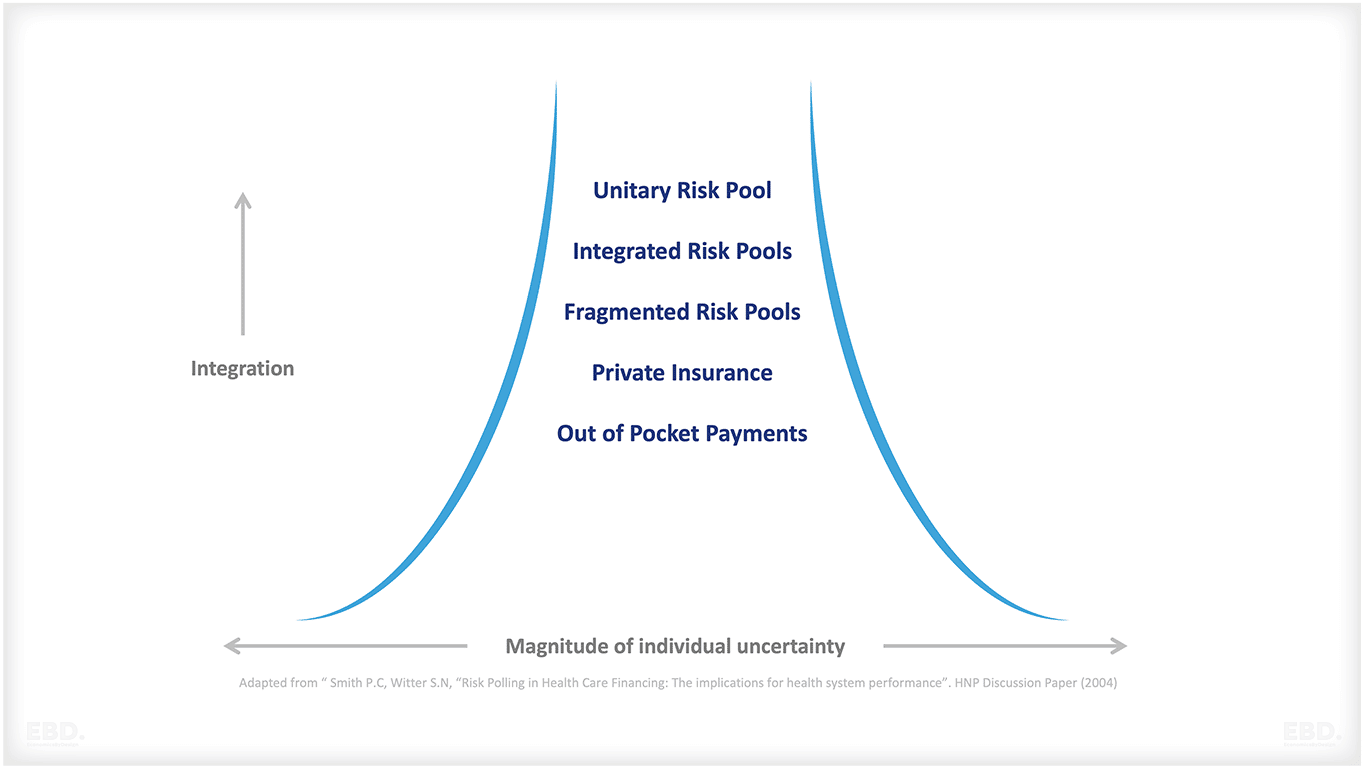
Smith et al (2004) set out four classes of risk pooling:
No Risk Pooling
This is where each person pays for their own health care needs and all liability lies with the individual.
Unitary Risk Pooling
This is where all health risks for a population are pooled together in a single national fund.
Fragmented Risk Pooling
These are a series of independent risk pools for different population groups.
Integrated Risk Pooling
These are where financial transfers are made across fragmented risk pools to mitigate the health inequalities and risks of poor financial protection which arise from fragmented risk pooling.
Risk pooling can be based on equal contributions enabling a transfer from the well to the sick. Or they can also be based on income-related contributions which often enable redistribution from the wealthier to the poorer members.
Contributions can also be based on employment, enabling a redistribution from those who are able to work to those who are not. It can also help those who may face higher health risks on account of age for example.
How Does Risk Pooling Vary Across the World?
There is no one-size-fits-all approach to risk pooling and the way in which it is implemented varies across the world. In some countries, risk pooling is done through a unitary system where all risks are pooled together in a single national fund. In other countries, risk pooling is done through a fragmented system where there are a series of independent risk pools for different population groups.
Risk Pooling in High-Income Countries
In high-income countries, it is common to see unitary risk pooling or integrated risk pooling of some form. Even in the USA, risks can be pooled based on income (Medicaid), age (Medicare and the Children’s Health Insurance Program) and employment (with integration supported by the Affordable Care Act).
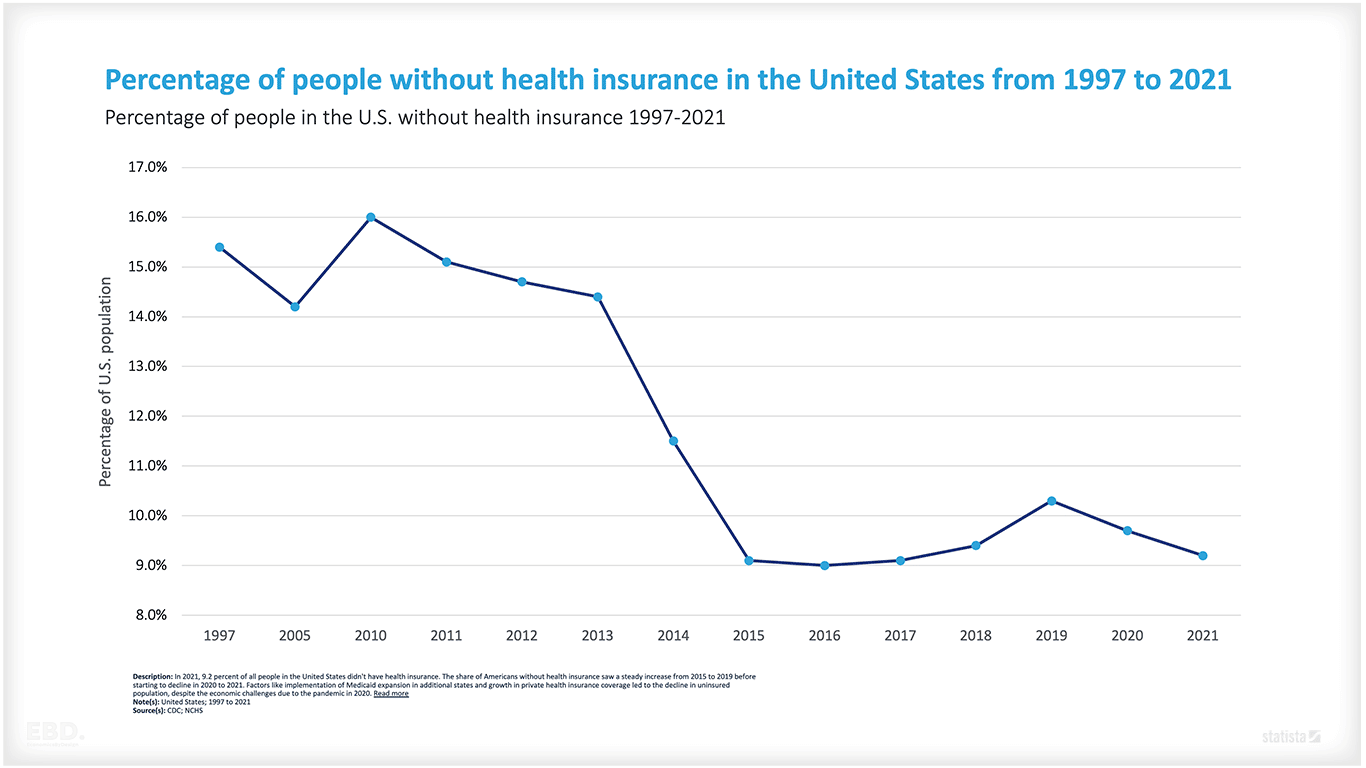
Despite this, the USA still does not have Universal Health Coverage with just above 9% of the population still uninsured (2021).
Risk Pooling in Low/Middle-Income Countries
Risk pooling in low and middle-income countries (LMICs) can take a variety of forms. In some cases, there may be no risk pooling at all with each individual responsible for their own health care needs. In other cases, there may be fragmented risk pooling with a series of independent risk pools for different population groups.
In other cases, there may be some form of integrated risk pooling where financial transfers are made across fragmented risk pools to mitigate the health inequalities and risks of poor financial protection, which arise from fragmented risk pooling.
Risk Pooling and Universal Health Coverage
Risk pooling is an important part of achieving Universal Health Coverage (UHC) as it helps to ensure that everyone has access to the health care they need, regardless of their ability to pay.
Options for improving risk pooling include:
Increasing the level of risk pooling:
This can be done by increasing the number of people who are covered by a given risk pool, by increasing the size of the risk pool itself, by merging or cross-subsidizing fragmented risk pools, or by making coverage compulsory.
Improving the design of risk pools:
This can be done by ensuring that risk pools are well-designed, harmonized and efficient in order to make the best use of resources.
Improving how risks are pooled:
This can be done by ensuring that risks are pooled and benefits redistributed in a way that is equitable, efficient, sustainable, and effective.
What are the Challenges of Risk Pooling?
One challenge relates to an effect known as Moral Hazard. This occurs when people are insulated from the consequences of their actions. For example, if you have health insurance and know that your medical bills will be covered, you may be more likely to visit the doctor or alternatively take risks with your health.
Moral hazards can lead to higher health care costs as people use more health care services than they would if they were paying out-of-pocket. It can also lead to a deterioration of health as people take risks that they would not otherwise take.
There are several ways in which moral hazards can be minimized:
By ensuring that people are invested:
This can be done by requiring people to make a co-payment for health care services or by making them responsible for a certain amount of their health care costs.
By designing incentives carefully:
This can be done by aligning incentives so that people are rewarded for healthy behaviour or penalized for unhealthy behaviour.
By providing information:
This can be done by informing people about the risks of certain behaviours and the consequences of their actions.
A further challenge occurs when the pooling includes small predictable expenses that shouldn’t really be included (such as insured access to low-cost pharmaceuticals for common conditions such as the common cold). This increases the costs associated with risk pooling compared to the benefit.
Other challenges relate to the relationship between contribution and coverage. Should contributions be based on families, households, or individuals? How should prior conditions be dealt with fairly and equitably?
The biggest challenge of all is creating a pool big enough to cover the risks. This analysis is usually done by actuaries. An actuary is a business professional who deals with the measurement and management of risk and uncertainty. Actuaries use their knowledge of mathematics, statistics, economics, and finance to calculate the probability and expected costs of events such as death, injury, and disease, natural disaster. Actuarial skills are in relatively short supply but are essential for risk pooling.
How Does Risk Pooling Impact the Economy?
Risk pooling can have a positive impact on the economy by helping to reduce the financial burden of health care on individuals and families. This, in turn, can free up money that can be spent on other goods and services, which can boost economic growth.
In addition, risk pooling can help to improve access to health care, which can lead to better health outcomes and increased productivity.
Finally, risk pooling can help to improve the quality of health care, as it provides an incentive for providers to invest in research and development to find new and better ways to treat and prevent disease.
Copyright © 2022 – Economics By Design. All rights reserved