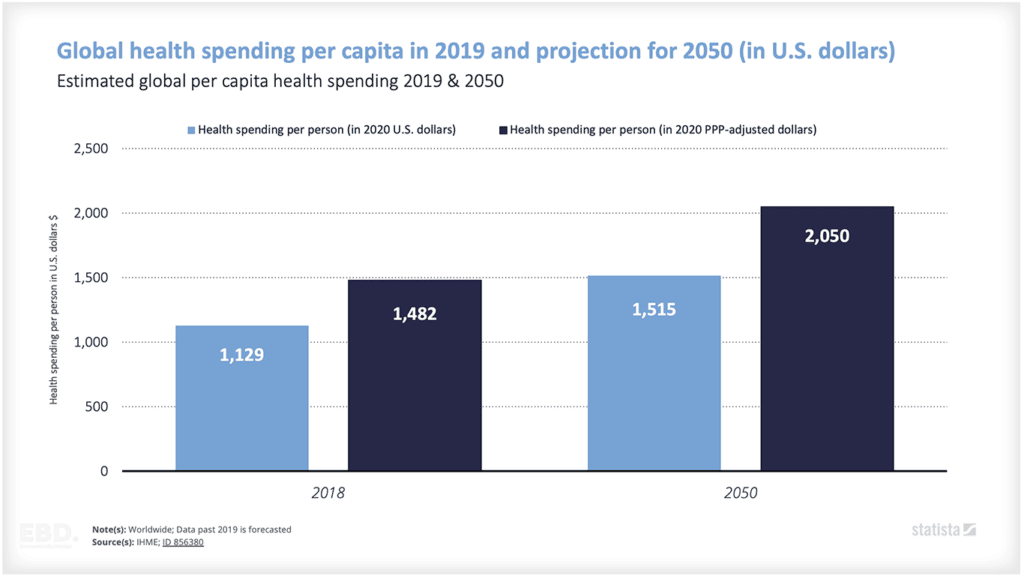
The terms healthcare workforce or healthcare professionals cover a vast array of disciplines and professional practices. There are over 350 different health careers including medical, nursing, allied health professionals, scientific, and managerial.
Increasingly health professionals work in multi-disciplinary or multi-professional teams and, as workforce training and skills development evolve, many are now able to extend their traditional scope of practice by through enhanced or advanced practice roles.

This economic lens provides an overview of the different types of healthcare professional. It does not cover social care although increasingly care workers are included as part of multi-disciplinary teams supporting people with rehabilitation and providing long-term care for those who need it.
Doctors
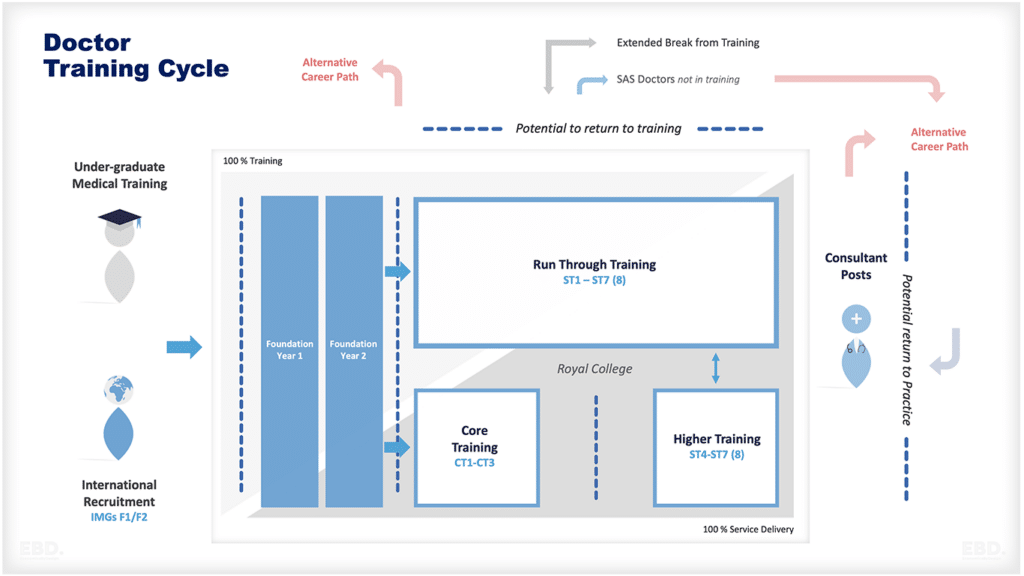
Physicians, surgeons, general practitioners, and dentists are key members of the medical profession. All must be qualified to practice in their particular field and have completed a recognised medical degree, usually at a medical school hosted by a university. It can take up to seven years to graduate from medical school and arrangements are different across different countries.
Post graduation, there is a period of training as a front-line clinician and this can take a further 10 years depending on how much an individual chooses to specialise and what is required by the relevant professional body in the country. The World Federation for Medical Education provides guidance on the standards for the development and evolution of medical education programmes; these are used by around half of medical schools globally.
Health services are organised around clinical specialities and doctors tend to specialise in a particular speciality area. The figure below shows the share of specialities of doctors based in the United Kingdom in 2021.
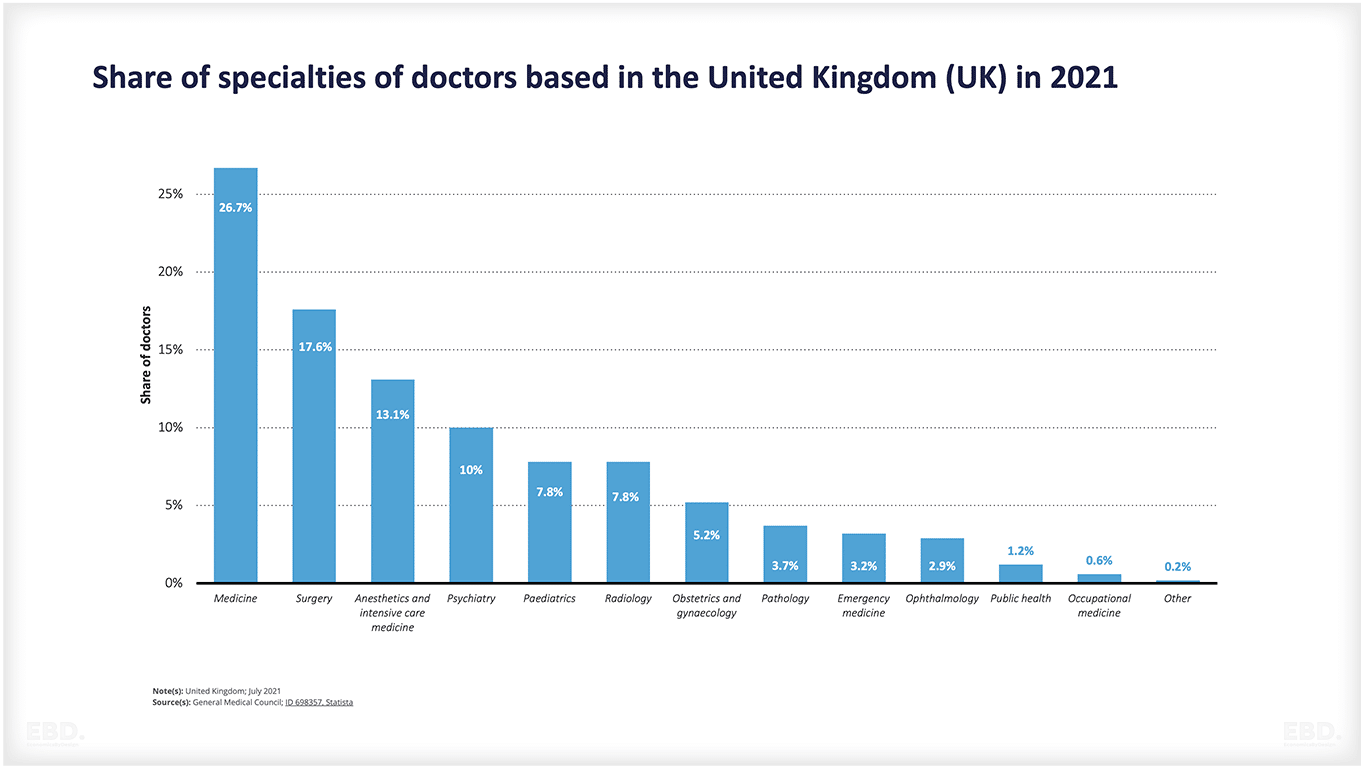
Generally, doctors are responsible for diagnosing illnesses, prescribing treatments/medications and referring patients to other specialists if required. Surgeons perform operations or other invasive surgical procedures.
Other examples of medical professionals include
- Anaesthetists who provide anaesthetics to patients when they are undergoing procedures and also provide pain relief to patients when needed
- Radiologists who use images to help diagnose, treat and manage patients with health conditions
- Pathologists who specialise in diagnosis based on a detailed examination of blood, cells and body tissue
- Public Health doctors who support public health and prevention programmes.
Doctors are generally regulated by a nominated country’s regulatory authority. These vary country by country but the goal is to ensure that registered practitioners are fit-to-practice and can be trusted by patients and other stakeholders across the healthcare system as having the necessary qualifications, skills and experience for the role they have.
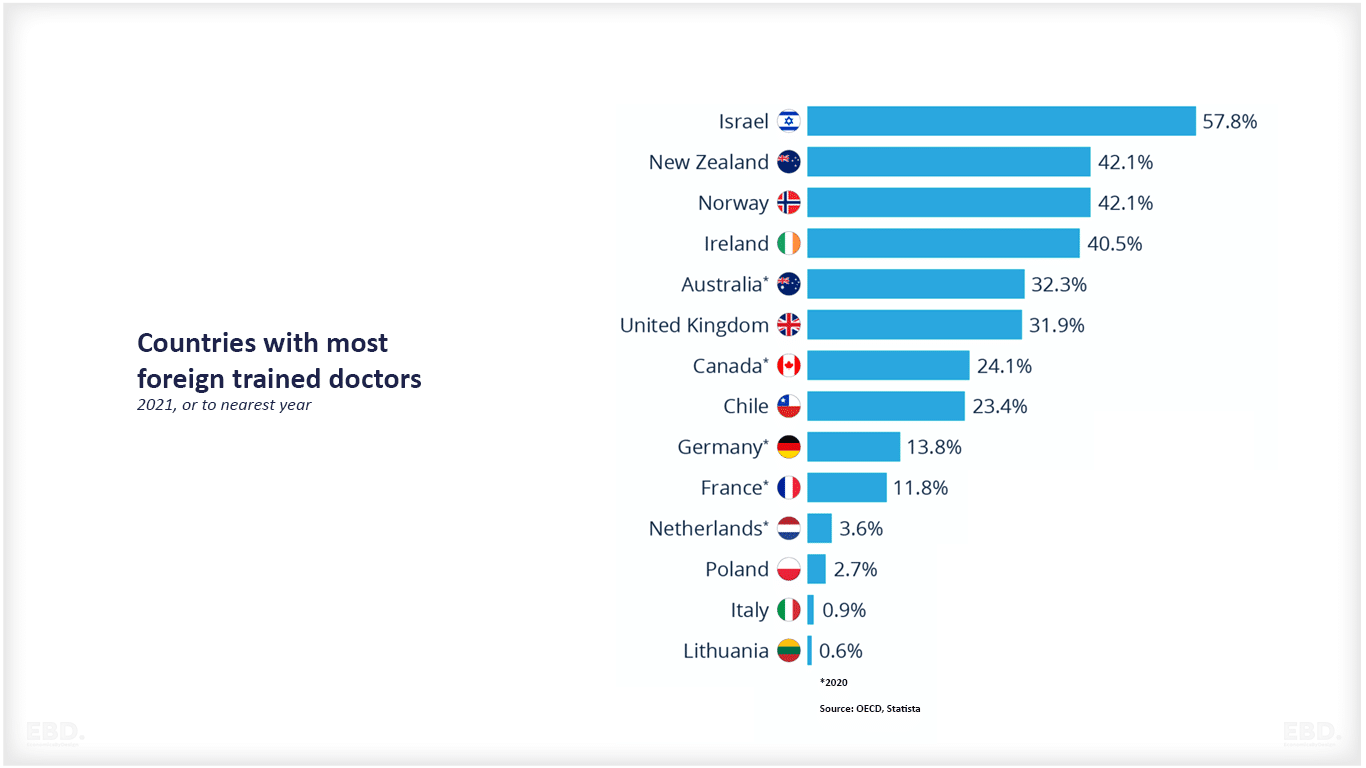
Doctors often work overseas for a period of their career. The chart below shows the share of doctors who were foreign trained for selected OECD countries.
Italy has very few foreign trained doctors at less than 1%, whereas in Israel well over half of all doctors (57.8%) are foreign trained.
Dentists
Dentists diagnose, treat and prevent diseases of the teeth, gums and mouth, fill cavities, extract teeth, place crowns or bridges and provide advice on oral hygiene. Dentists usually need to undertake a university degree and gain clinical experience to gain a license to practice. Depending on the country they will also need to be regulated by an appropriate regulatory body.
Nurses
The International Council of Nurses define nursing as follows:
“Nursing encompasses autonomous and collaborative care of individuals of all ages, families, groups and communities, sick or well and in all settings. Nursing includes the promotion of health, prevention of illness, and the care of ill, disabled and dying people. Advocacy, promotion of a safe environment, research, participation in shaping health policy and in patient and health systems management, and education are also key nursing roles “(ICN, 2002)
Nurses usually need to earn a degree in nursing and pass an exam before they can be registered as a nurse. All countries have different requirements and these are managed by the relevant professional body or ministry of health. In some cases, nurses may also choose to specialise their practice within certain areas such as theatre nursing, paediatrics, geriatrics, mental health, district nursing, health visitors etc.
Nurses are also regulated by a nominated country regulatory authority to provide assurance that they are able to deliver the services commensurate with their role.
In some countries, nurses have been able to acquire advanced practice skills and are able to prescribe medication, perform surgical procedures, and other services traditionally outside their scope of practice.
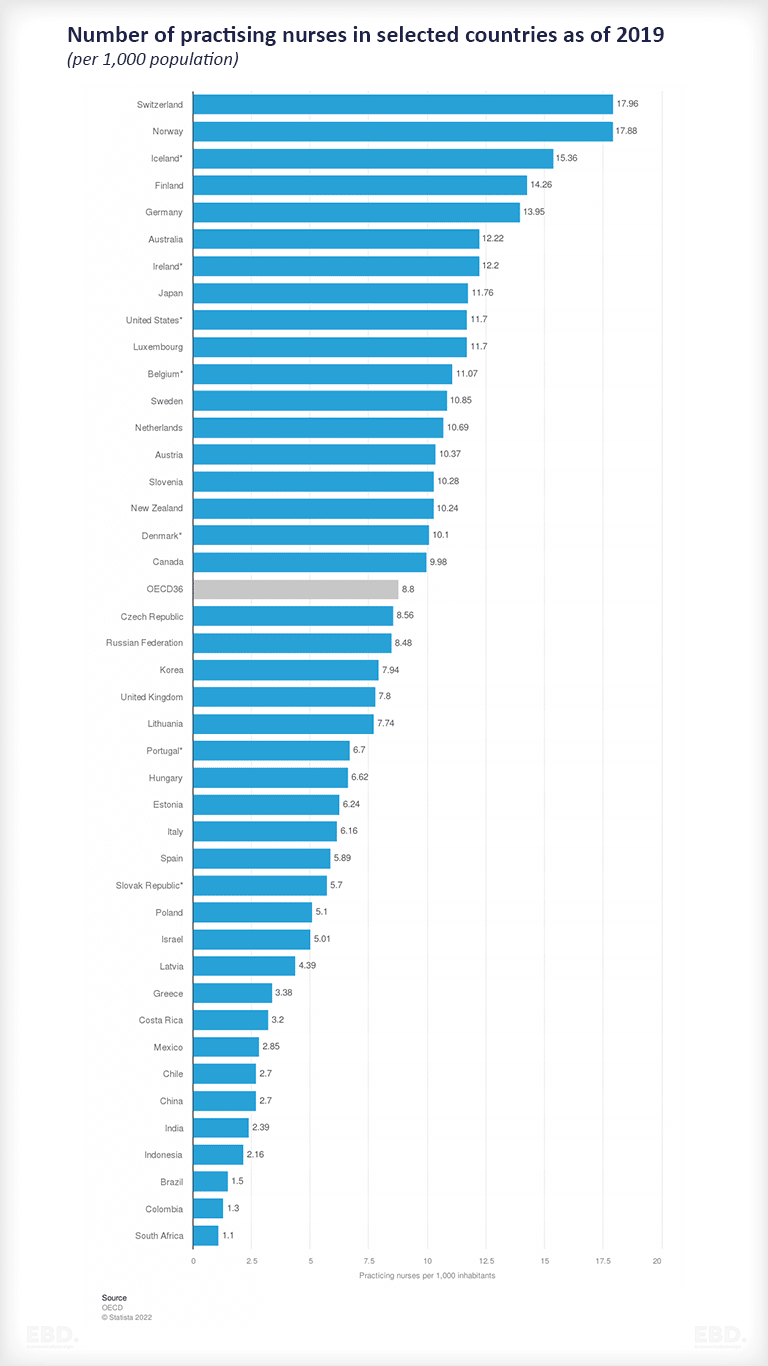
There is considerable variation in access to nursing staff by country. The chart below shows the number of practising nurses per 1,000 inhabitants across the OECD in 2019.
Midwives
Midwives provide care from pregnancy through to the birth and postnatal period, assisting women with labour and delivery, providing antenatal and postnatal support, family planning advice and promoting a healthy lifestyle. As with nursing, midwives generally require a university degree and clinical practice experience to be registered to practice.
Midwifery is a regulated profession in most countries and midwives are required to meet certain qualifications before they can be registered to practice. In some countries, midwives have increased their scope of practice, to include prescribing medications and treatments, pain control medications and birth control.
Pharmacists
Pharmacists provide advice about medicines including how to take them safely and effectively. Generally, they need to have a degree or post-graduate degree in pharmacy plus post-graduate clinical experience before they can be registered to practice. Pharmacists are often supported by pharmacy technicians who also need to meet qualification standards to be registered to practice.
Generally a doctors role will be to prescribe medication and a pharmacists role will be to advise on drugs and dispense medications to patients. However, in some countries, pharmacists are increasing their scope of practice to include delivering vaccines, prescribing medications, taking blood pressure, and delivering prevention services such as smoking cessation, weight management etc.
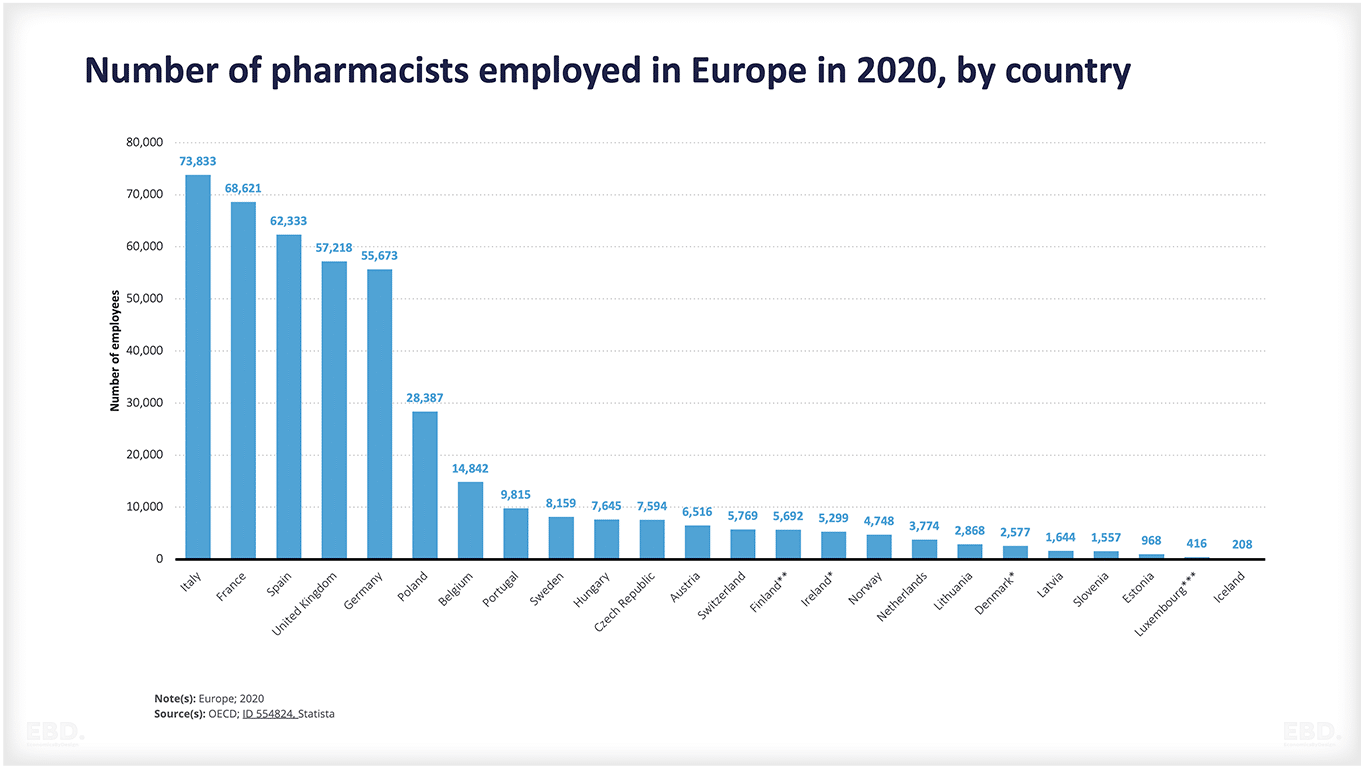
The chart below shows the number of pharmacists employed in the health sector in Europe in 2020.
Other “Allied” Health Professionals
The term Allied Health Professionals is an umbrella term sometimes used to describe a range of other health professionals that work with doctors and nurses to support prevention, treatment and care for the population and for patients.
Here are just some examples:
- Physiotherapists who assess, diagnose and treat physical problems or impairment caused by illness, injury or disabilities
- Occupational therapists help people to regain their independence after illness or injury
- Radiographers who operate imaging technology to support diagnosis and condition management. In some countries, radiographers can also be trained to report imaging results (reporting radiographers).
- Speech and language therapists help people with speech, language, swallowing and communication difficulties.
- Art therapists work with individuals using a range of art media to help them cope with mental health issues
- Drama therapists enable people to explore their inner feelings and emotions in a safe environment.
- Music therapists who use music to help improve cognitive, emotional and physical health.
- Chiropodists / podiatrists provide assessment, diagnosis and treatment of foot problems.
- Nutritionists/dietitian advise people on diet to help prevent or manage medical conditions.
- Paramedics provide pre-hospital treatment and support for people with life threatening illnesses or injuries.
- Orthoptists diagnose and treat disorders of the eye muscles. They will often work with Ophthalmologists, surgeons who are able to support patients with diseases of the eyes and who undertake surgical interventions and prescribe a wider range of treatments.
- Osteopaths use physical manipulation, stretching and massage to treat musculo skeletal problems.
- Prosthetists / Orthotists design, create and fit artificial limbs and braces to help people with mobility issues.
- Operating department practitioners support the theatre team in the operating department for patients undergoing surgery.
- Healthcare scientists use laboratory tests and advanced technology for the diagnosis and monitoring of diseases
- Clinical psychologists provide psychological therapies to help people manage mental health issues.
- Counsellors help people with a range of emotional and mental health needs.
Many of these health professionals need to have a degree or postgraduate qualification in the field that they wish to practice in although regulations and standards vary country by country.
The role of other health professionals is changing in response to the increasing demand for integrated primary care and community services.
For example, in some countries, registered Allied Health Professionals are now employed as part of multi-disciplinary teams, working alongside doctors and nurses to provide comprehensive patient care. As with the other regulated professions, some countries are enabling these staff to extend and expand their scope of practice through new Enhanced and Advanced Practice roles.
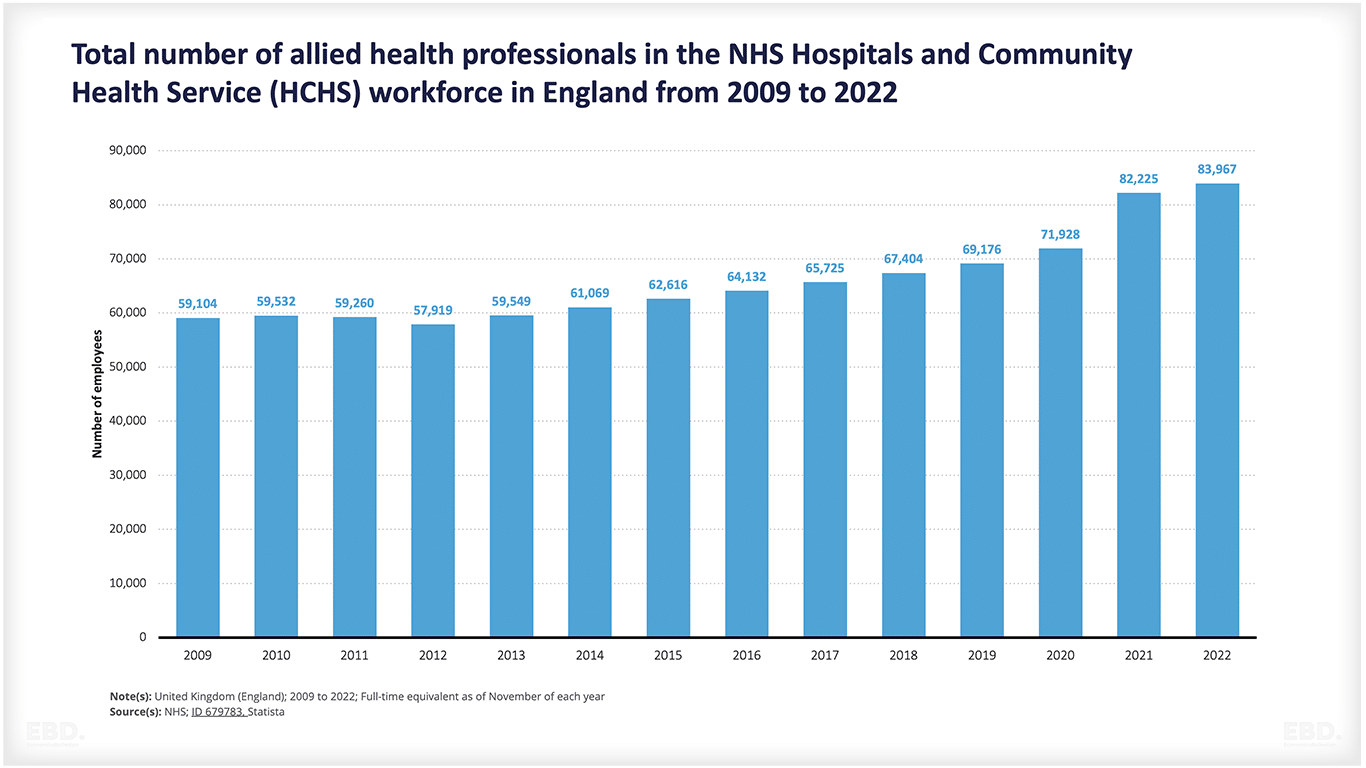
The chart below shows how these professions have grown in the NHS in England since 2009. Note that of the list given above, this chart excludes clinical psychologists, counsellors, and clinical scientists.
Health Managers + Administrators
In addition to the clinical roles of doctors, nurses and Allied Health Professionals, health systems employ a range of managers and administrators. Their role is often essential for the successful running of a health service. They are responsible for leadership and management, human resources, budgeting and financial management, policy development, IT/data security and communication with other stakeholders.
The Global Shortage of Health Workers
The World Health Organisation is currently projecting a shortage of 10 million health workers by 2030, with shortages particularly severe in low and middle-income countries.
Healthcare systems can’t function without the health workforce and universal health coverage is being held back for want of investment in education, training, and funding to pay salaries commensurate with the human capital investment required of health workers themselves.