
Health Financing
Health financing is a critical enabler of Universal Health Coverage (UHC). It ensures that people can access the universal coverage for health services they need without suffering financial hardship.
There are many different ways to flow funds through the health care system, but all systems have four basic elements:
Financing & Revenue Sources
This is when funds are gathered from people to pay for health care needs. This can be done at scale through government contributions, taxes, social insurance contributions, private insurance contributions, or philanthropic contributions. It also includes out-of-pocket payments by individuals paying directly for treatment when it is needed.
Risk Pooling
Funds gathered at scale can be pooled together in a way that allows them to be used more efficiently and effectively. This means that the risks of needing healthcare are shared among a larger group of people, which helps to keep costs down. Pooling can be done through a single fund for a whole health system, regional funds for sub-national systems, or multiple funds for specific population groups.
Strategic Purchasing
Pooled funds are used to purchase health care services for a group. This can be done directly by the government or through private insurers. It includes making contracts with providers, setting prices, and ensuring that quality standards are met.
Provider Payment Models
Providers (such as hospitals and doctors) need to be paid for the health care services they provide. This can be done through a variety of models, capitation, block funding, line-item funding, fee-for-service, case-based payments, or a mix of some or all. It can include incentives to improve performance or conditional on achieving pre-agreed outcomes.
The focus of this economics lens is on the financing and revenue sources.
How Is Healthcare Financed?
There are many different ways to achieve Universal Health Coverage, but all require a mix of financing mechanisms. The most common way to finance health care is through a mix of public and private sources.
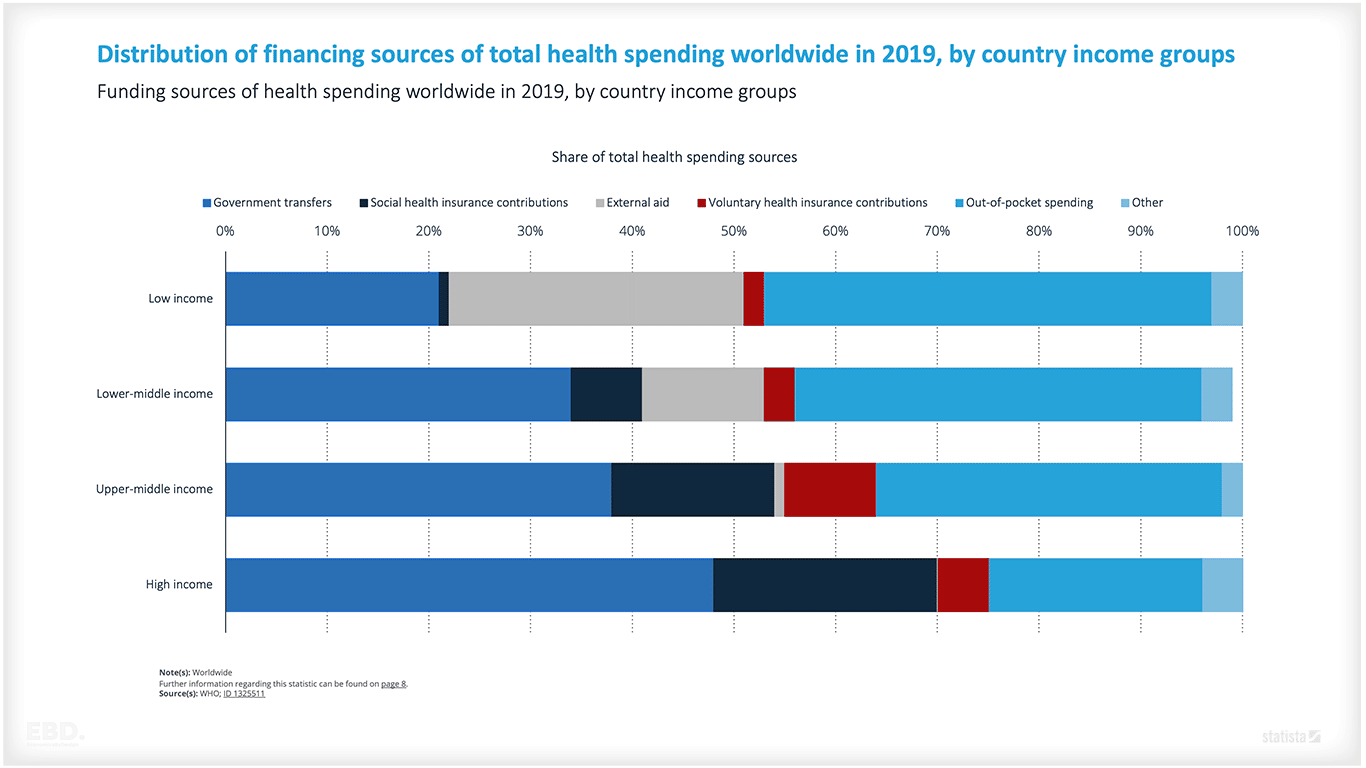
General Taxation + Government Transfers
This is the most common method of health financing in high-income countries. Taxes can be used to finance healthcare directly, or they can be used to co-fund social health insurance programs.
Examples of countries using general taxation to finance all or part of their healthcare system include:
- Australia
- Canada
- France
- Germany
- Japan
- New Zealand
- United Kingdom
- United States of America
Social Health Insurance
Social health insurance is when people contribute to a pool of funds that is used to pay for healthcare services. In many countries, social health insurance is mandatory for all citizens or residents. This is another common method of health financing in high-income countries.
Examples of countries using social health insurance include:
- Belgium
- Denmark
- Finland
- Hungary
- Italy
- Holland
- Norway
- Portugal
- Spain
- Sweden
- Switzerland
External Aid + Philanthropy
This is when people or organizations donate money or resources to support healthcare services. This is an important source of health financing for many healthcare organizations, especially in low- and middle-income countries.
Examples of healthcare organizations that rely heavily on philanthropy include Médecins Sans Frontières (MSF, or Doctors Without Borders), the Global Fund to Fight AIDS, Tuberculosis and Malaria, and the Bill & Melinda Gates Foundation.
Voluntary Health Insurance
This is when people purchase insurance schemes voluntarily. This is often from a private company to cover healthcare costs. This method of health financing is common in countries with a mix of public and private healthcare and is used proportionately more in upper-middle income countries than elsewhere.
Examples of countries using private health insurance include:
- Chile
- Colombia
- Costa Rica
- Ecuador
- Mexico
- Peru
Out-of-pocket Payments
This is when people pay for healthcare services directly from their own pockets. This is often done for services that are not covered by social health insurance.
According to data from the World Bank, out-of-pocket spending has fallen globally from 19.28% of total spending to 18.01% (2019). However, some countries have very high levels with Armenia, Afghanistan, Turkmenistan, Myanmar and Equatorial Guinea having over 75% of health spending financed by out-of-pocket payments.
Using Finance To Classify Health Systems
There are three common healthcare system models which combine these health financing models and are often used to classify health systems.
The Beveridge Model
The Beveridge Model, named after Sir William Beveridge, also known as the National Health Service (NHS) model, is a healthcare system where healthcare is provided by the government and funded by taxation. This system is common in many European countries such as the United Kingdom, France, Spain, and Portugal.
In this model, health care is available free at the point of use. This can result in patients overutilizing the health system but this risk is usually managed through pro-active prevention programmes, and the use of primary care and effective triage to select patients for treatment in order of priority. This helps to manage demand across the system.
The Bismarck Model
The Bismarck Model, named after Otto von Bismarck, also known as the Social Health Insurance (SHI) model, is a healthcare system where healthcare is provided by the government and funded by social health insurance contributions. Some of these systems have many insurers but the prices and health benefit packages are heavily regulated or managed by the government.
This system is common in many European countries such as Germany, Belgium, and Switzerland. This system works well for the employed but it requires a financial ‘safety net’ for unemployed, retired and other citizens who are unable to afford contributions.
The National Insurance Model
The National Insurance Model, also known as the mixed public-private model, is a healthcare system where healthcare is provided by both the government and private sector. In general, however, the financing comes from government-run insurance programmes that every citizen contributes into.
This model uses elements from both the Beveridge and Bismarck models, aiming to balance the public and private health provision.
This system is common in many countries such as Canada, and the United States of America (Medicare). These systems can result in high costs and long waiting times, and the complex and varied arrangements with private providers can result in poor care coordination and patient responsiveness; although this is not a result of the financing itself.
Why Can’t We Rely On Out-of-Pocket Payments to Finance Health Care?
There are several challenges associated with financing healthcare solely through out-of-pocket payments:
Catastrophic Health Spending
This is when health care costs exceed what a household can afford to pay. This can lead to financial hardship and even poverty. The World Health Organisation and the World Bank Monitoring Report on Financial Protection 2021, report catastrophic health spending using two thresholds; when out-of-pocket expenditure is above 10% or 25% of household income. Some studies have used different indicators for example where out-of-pocket spending is above 40% of non-food consumption.
The table below shows that the size of the population facing catastrophic health expenditure was increasing even before the COVID-19 Pandemic.
Impoverished Health Spending
This is when healthcare costs push a household into poverty. This occurs when out-of-pocket healthcare expenditure exceeds a household’s capacity to pay, and they are forced to use other means, such as selling assets, to pay for healthcare.
As with catastrophic health spending, the incidence of impoverishing health spending is increasing. The numbers impoverished by out-of-pocket health spending have increased from 91m in 2002 to 172m in 2017.
Systems that over-rely on out-of-pocket payments for health financing are likely to experience increased health inequality, poverty, and relatively poor health outcomes.
Sustainability
Healthcare systems need to be sustainably financed to be sustainable in the long run. This means ensuring that there is a steady and adequate flow of resources to cover healthcare costs. Healthcare systems that are over-reliant on out-of-pocket payments are not sustainable because they rely on people being able to pay for healthcare services when they need them.
Why Can’t We Rely Solely On Private Health Insurance to Finance Health Care?
Countries with mature health insurance models such as the United States of America have a plethora of choices available to citizens in terms of health plans, however these benefits these come at a high price.
Healthcare coverage plans can vary in terms of:
- The level of deductibles (the amount of money that a person has to pay out-of-pocket before their insurance coverage starts)
- The level of co-payments (the fees that a person has to pay for healthcare services, even after their insurance coverage has started)
- The availability of catastrophic expenditure protection
- The choice of provider system
- What doctors the individual can see
The market for health insurance is significant and global.
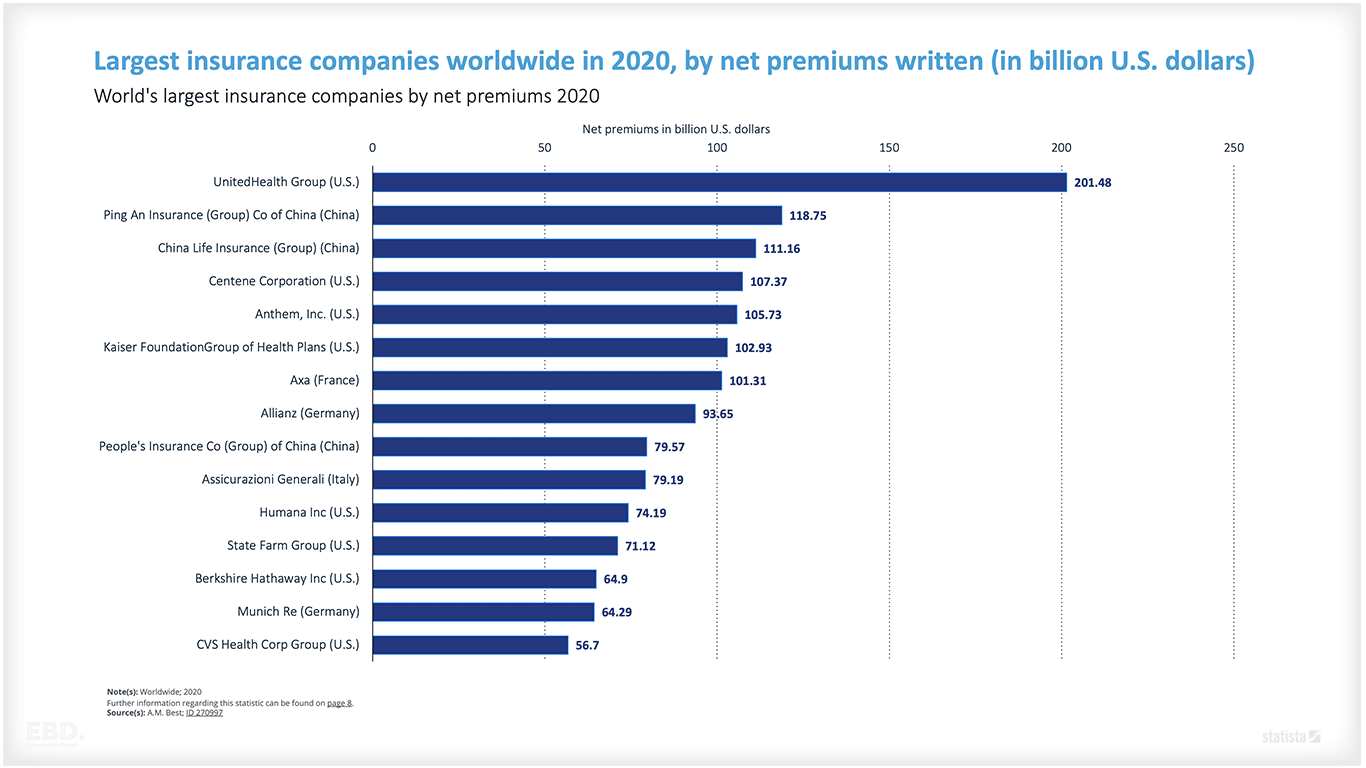
- UnitedHealth Group (U.S.) $201.48bn
- Ping An Insurance (Group) Co of China (China) $118.75bn
- China Life Insurance (Group) (China) $111.16bn
- Centene Corporation (U.S.) $107.37bn
- Anthem, Inc. (U.S.) $105.73bn
- Kaiser FoundationGroup of Health Plans (U.S.) $102.93bn
- Axa (France) $101.31bn
- Allianz (Germany) $93.65bn
- People’s Insurance Co (Group) of China (China) $79.57bn
- Assicurazioni Generali (Italy) $79.19bn
- Humana Inc (U.S.) $74.19bn
- State Farm Group (U.S.) $71.12bn
- Berkshire Hathaway Inc (U.S.) $64.9bn
- Munich Re (Germany) $64.29bn
- CVS Health Corp Group (U.S.) $56.7bn
What are the challenges with health insurance?
There are challenges with health insurance, which can make it difficult for everyone to obtain and maintain coverage. These challenges include:
The cost of premiums
Health insurance premiums can be very expensive, especially for those on low incomes. This can make it difficult for people to afford coverage.
The cost of deductibles and co-payments
Deductibles and co-payments can also be very expensive, which can make it difficult for people to afford healthcare.
Pre-existing conditions
People with pre-existing medical conditions often have difficulty obtaining health insurance coverage. This is because insurance companies may view them as being too high-risk and therefore not worth insuring.
Access to healthcare
Even if people have health insurance, they may not have access to healthcare. This is because there may not be any healthcare providers in their area who accept their insurance.
Cancellation of coverage
Health insurance companies can cancel people’s coverage if they get sick or have an accident. This can leave people without healthcare and struggling to pay medical bills.
Health insurance coverage can also simply expire, which can leave people without healthcare. This can be a problem for people who have chronic conditions or who need ongoing treatment.
Why Can’t We Rely Solely On Government Funding For Health Financing?
The cost of healthcare
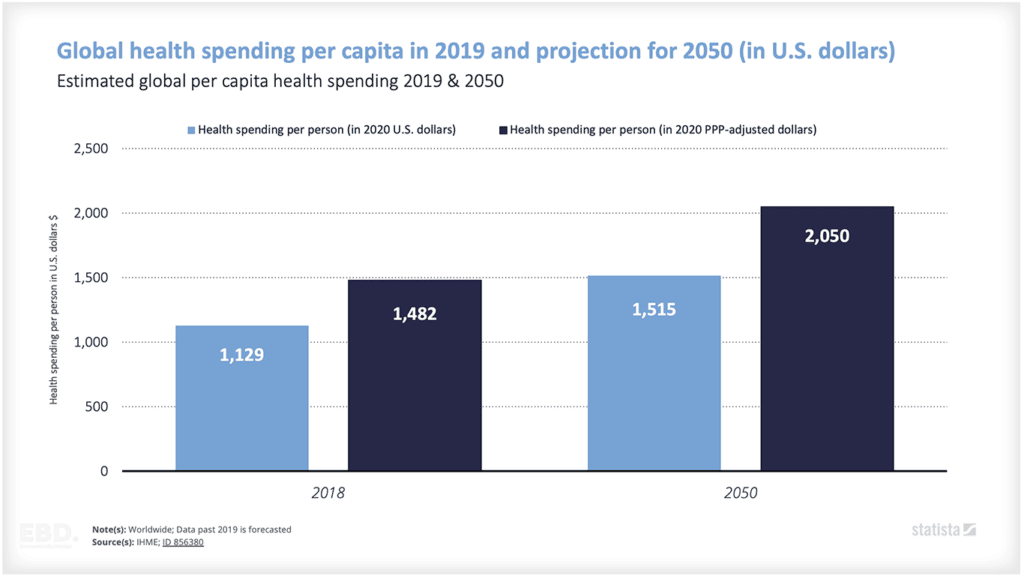
The cost of healthcare is constantly increasing, which can make it difficult for governments to keep up with the funding needs of healthcare systems. Healthcare costs increase as the population grows and life expectancy increases, new treatments become available, and consumer expectations rise.
Economic downturn
During times of economic downturn, government revenues decline. This can make it difficult for healthcare systems to maintain their current level of government funding. Government funding also has to compete with other government spending priorities such as defence, education, police and criminal justice, and critical infrastructure.
In low-income countries, high levels of local inflation can also reduce the government’s ability to secure international supplies of drugs and other health service consumables.
Political instability
Political instability can also lead to healthcare funding being cut or redirected to other areas. This can make it difficult for healthcare systems to function properly. Countries in fragile or conflict-affected settings often find themselves reliant on funding from international agencies, governments of other countries, or philanthropic organisations. These donor agencies may only have the scope or authority to fund specific programmes or emergency health services.
What Are The Potential Benefits Of A Mixed System of Health Financing?
Mixed health financing systems, which combine private and public sources of funding, can offer benefits.
Increased access to healthcare
Mixed health financing systems can increase access to healthcare by providing people with a choice of how to finance their healthcare. This can make healthcare more affordable for people who might not be able to afford it otherwise.
Increased choice of healthcare providers
Mixed health financing systems can also increase the choice of healthcare providers by allowing people to choose from a range of private and public healthcare providers. This can make healthcare more accessible for people who might not be able to access it otherwise.
Improved quality of healthcare
Mixed health financing systems can also improve the quality of healthcare by providing people with a choice of healthcare providers. This can allow people to choose healthcare providers who offer the best quality of care.
Increased efficiency
Mixed health financing systems can also increase the efficiency of health systems by allowing some healthcare providers to compete for patients. This can lead to healthcare providers offering more efficient and effective care.
What Health Financing Is Recommended For Integrated Care Systems?
There is no one-size-fits-all answer to this question, as the best health financing system for integrated care will vary depending on the needs of the healthcare system and the population it serves.
Whilst a mixed system of health financing, which combines private and public sources of funding, might maximise revenue to support an integrated care system, the flow of funds through the system needs careful consideration if the goals of population health and integration are to be achieved.
Pooling, resource allocation, purchasing strategies, and provider payment mechanisms are all important levers for ensuring that the resources find their way to the right part of the system quickly and efficiently.



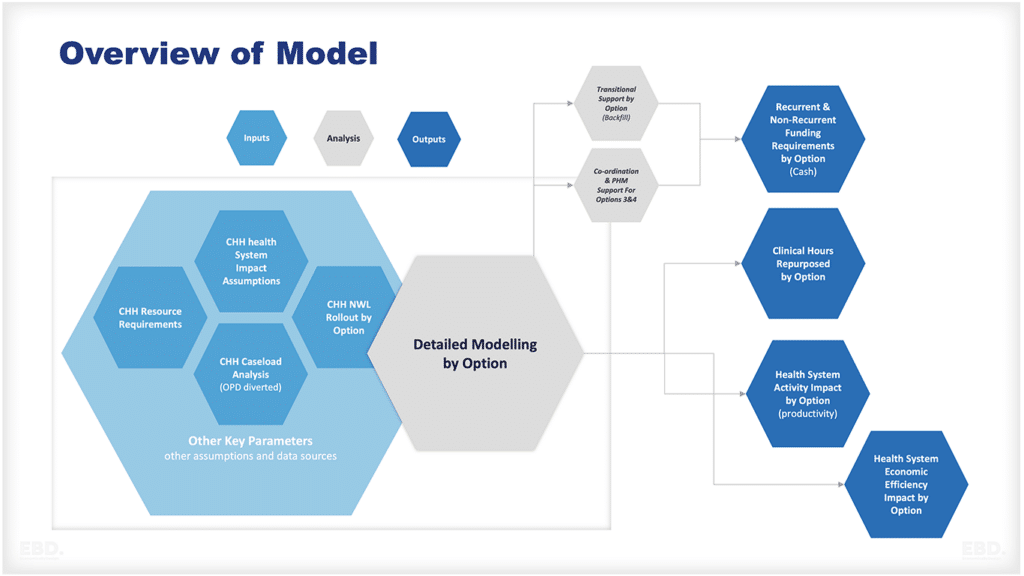
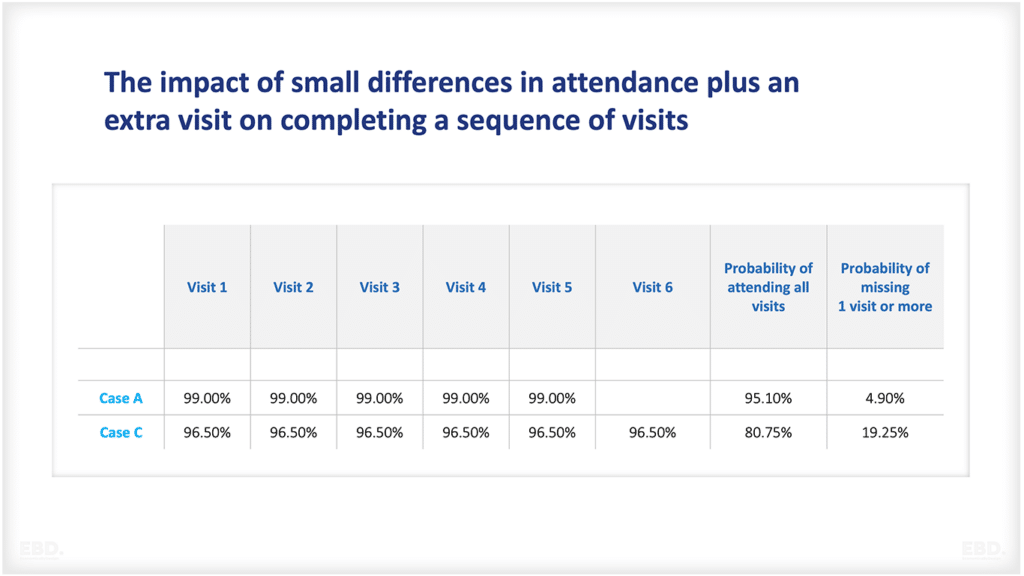













Very thorough and interesting. Thanks. An additional issue of concern with private health insurance centres on risk rating. As premiums become more subject to risk adjustment the effects of pooling are diminished. (In a sense, the logical end point of increased risk adjustment is self-insurance.) On the other hand, community rating, whereby uniform premiums are mandated, can lead to the so-called insurance ‘death spiral’ with a progressively smaller insured population of more risk-prone individuals who are obliged to pay higher premiums. Those at the lower end of the risk spectrum then become increasingly likely to drop their cover and the pool becomes even smaller, the average risk greater and premiums still higher … and so it goes on. Australia has worked quite creatively over many years to try to address this problem but still faces many challenges
Thanks so much for your thoughts Philip. I completely agree. Do take a look at the article on risk pooling.
Thank you very much. Clearly articulation of a topic that usually looses readers with its jargon!
Thanks Maria, appreciate your comment.