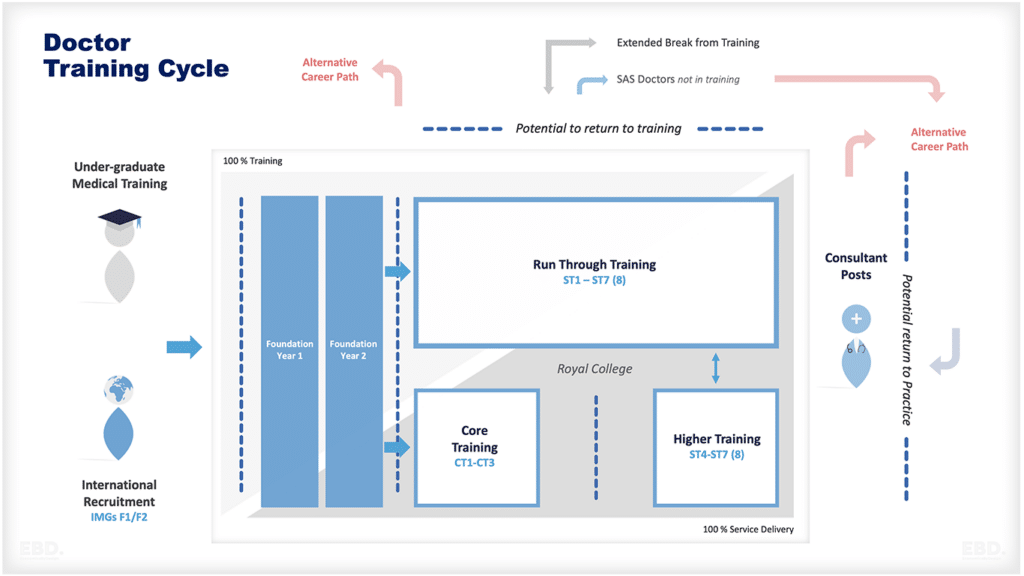
स्वास्थ्य पेशेवर
स्वास्थ्य पेशेवरों को प्रशिक्षित करना, भर्ती करना और अनुपस्थित होने पर कवर प्रदान करना महंगा है। यह लेख स्वास्थ्य प्रणाली के आर्थिक मूल्य और लागत को देखता है जब स्वास्थ्य पेशेवर स्वयं अस्वस्थ होते हैं।
22 मार्च में प्रकाशित 2021 एनएचएस स्टाफ सर्वेक्षण के परिणामों में कर्मचारियों के स्वास्थ्य से संबंधित कुछ दिलचस्प आंकड़े शामिल हैं [1]।
अन्य बातों के अलावा, प्रश्नावली ने बताया:
- 3 में से 1 से अधिक कर्मचारियों ने अपने काम के कारण जला हुआ महसूस करने की सूचना दी (एम्बुलेंस कर्मचारियों के आधे से अधिक)
- 30.8% कर्मचारियों ने काम की गतिविधियों के कारण मस्कुलोस्केलेटल समस्याओं का अनुभव किया
- पिछले 12 महीनों में काम से संबंधित तनाव के कारण 46.8% कर्मचारी अस्वस्थ महसूस कर रहे हैं
- 54.5% कर्मचारी अपने कर्तव्यों का पालन करने के लिए पर्याप्त महसूस नहीं करने के बावजूद पिछले 3 महीनों में काम पर गए हैं।
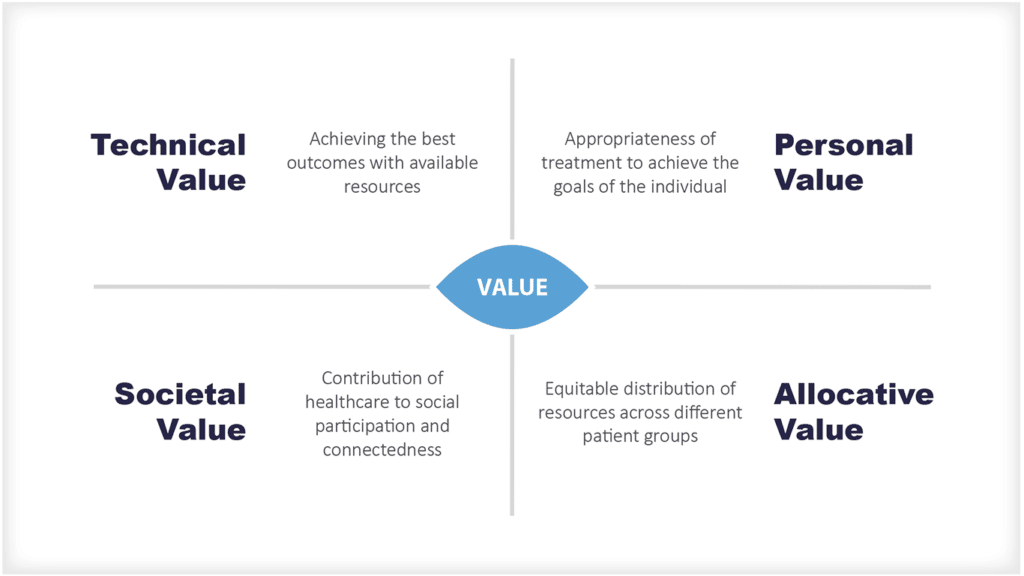
आर्थिक मूल्य
स्वास्थ्य अर्थशास्त्र के दृष्टिकोण से, ये बहुत महंगे आंकड़े हैं।
स्वास्थ्य पेशेवरों को प्रशिक्षित करने, भर्ती करने और अनुपस्थित होने पर कवर प्रदान करने के लिए महंगा है। जब मैं कर्मचारियों की भलाई की आर्थिक लागत के बारे में एनएचएस सहयोगियों से बात करता हूं, तो चर्चा का ध्यान अक्सर बीमारी की अनुपस्थिति, एजेंसी के कर्मचारियों का उपयोग करने की वैकल्पिक लागत, कवर के बिना मुकाबला करने, या चरम, कर्मचारियों के कारोबार पर होता है।
शायद ही कभी सहकर्मी बीमार होने पर काम पर आने वाले कर्मचारियों से जुड़ी लागत के बारे में बात करते हैं, और इसका प्रभाव उनकी काम करने की क्षमता पर पड़ता है। हम अर्थशास्त्री इसे "प्रस्तुतिवाद" कहते हैं।
प्रस्तुतिवाद की आर्थिक लागत है। उत्पादक समय का नुकसान रोगियों की देखभाल के मूल्य, देखभाल प्रदान करने वाले कर्मचारियों के अनुभव पर नकारात्मक प्रभाव डालता है, और स्वास्थ्य प्रणाली (नियोक्ता के रूप में) की लागत बढ़ाता है।
जनवरी 2020 में, डेलॉयट ने एक रिपोर्ट प्रकाशित की "मानसिक स्वास्थ्य और नियोक्ता: निवेश के लिए मामले को ताज़ा करना"[2]. रिपोर्ट में मानसिक स्वास्थ्य से संबंधित प्रस्तुतिवाद की लागत का अनुमान शामिल था। उन्होंने अनुमान लगाया कि प्रस्तुतिवाद की लागत ब्रिटेन के नियोक्ताओं को £ 26.6 बिलियन और £ 29.3 बिलियन प्रति वर्ष के बीच है। इसमें व्यक्तियों पर प्रभाव या नियोक्ता के दृष्टिकोण से, टीम वर्किंग शामिल नहीं था।
यह £ 6.8 बिलियन की अनुपस्थिति लागत और £ 8.6 बिलियन की टर्नओवर लागत के साथ तुलना करता है। वास्तव में, समग्र लागत में प्रस्तुतिवाद के प्रभाव सहित आर्थिक प्रभाव लगभग दोगुना हो जाता है।
डेलॉयट की रिपोर्ट में स्वास्थ्य क्षेत्र में मानसिक स्वास्थ्य से संबंधित प्रस्तुतिवाद, अनुपस्थिति और कारोबार की संयुक्त लागत के रूप में £ 1568 - £ 1840 प्रति कर्मचारी का अनुमान शामिल था। इसे डूबने दीजिए। संभावित रूप से यह अकेले एनएचएस कर्मचारियों में लगभग £ 2 बिलियन की लागत के बराबर है। यदि आप व्यापक स्वास्थ्य मुद्दों (जैसे मस्कुलोस्केलेटल समस्याओं) को शामिल करते हैं तो लागत बहुत अधिक होगी।
एनएचएस में कर्मचारियों की भलाई हब का विकास, जो समर्थन के लिए तेजी से पहुंच प्रदान करता है, एक बहुत ही स्वागत योग्य और संभावित उच्च मूल्य वाला निवेश है [3]। इनमें से 40 देश भर में स्थापित किए गए हैं और अब लाइव हैं।
यह देखना दिलचस्प होगा कि 54.5% कर्मचारियों द्वारा उनका कितनी अच्छी तरह उपयोग किया जाता है जो काम पर प्रस्तुतिवाद का अनुभव कर रहे हैं। यह और भी दिलचस्प होगा अगर हम खराब कर्मचारियों के स्वास्थ्य की आर्थिक लागत पर भलाई केंद्रों के प्रभाव को माप सकें।
[1] https://www.nhsstaffsurveys.com/results/national-results/
[2] https://www2.deloitte.com/uk/en/pages/consulting/articles/mental-health-and-employers-refreshing-the-case-for-investment.html
[3] https://www.england.nhs.uk/supporting-our-nhs-people/support-now/staff-mental-health-and-wellbeing-hubs/