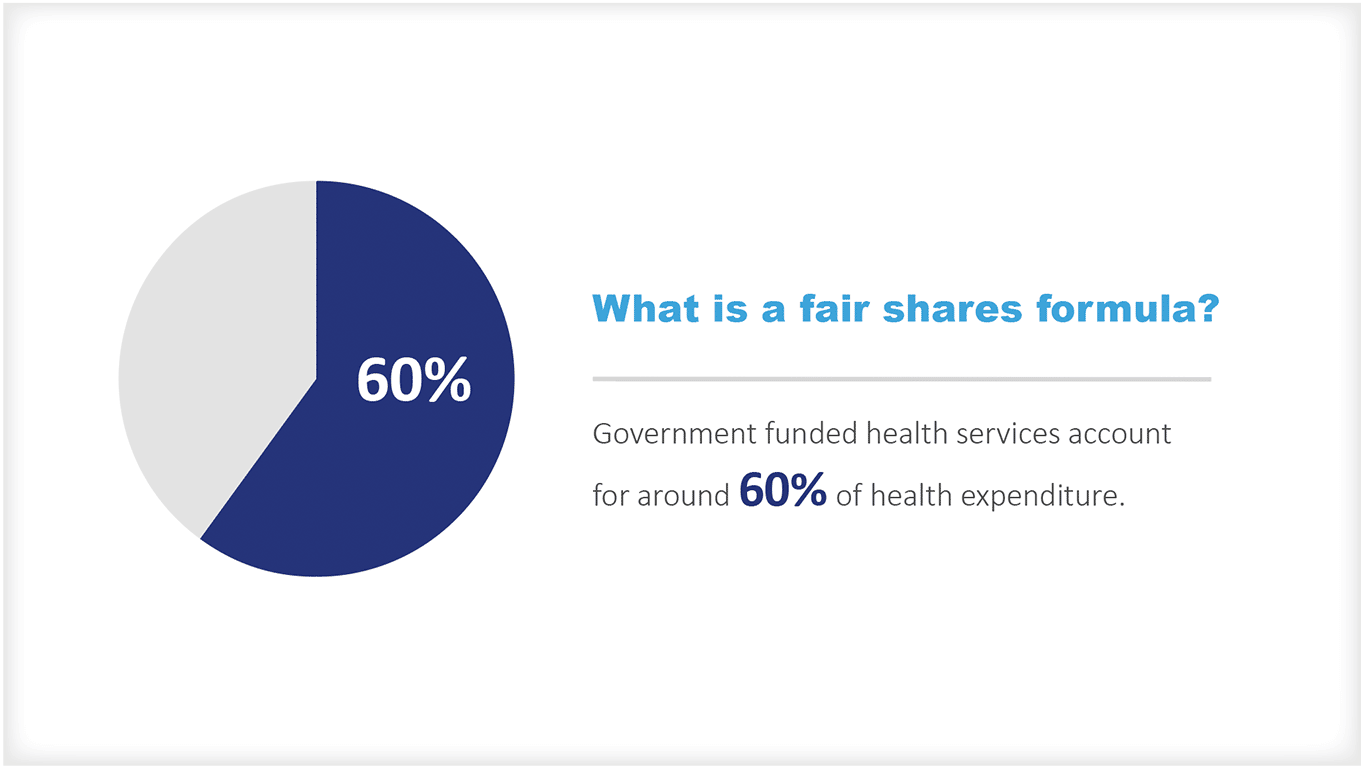
什么是公平份额公式?
资源分配
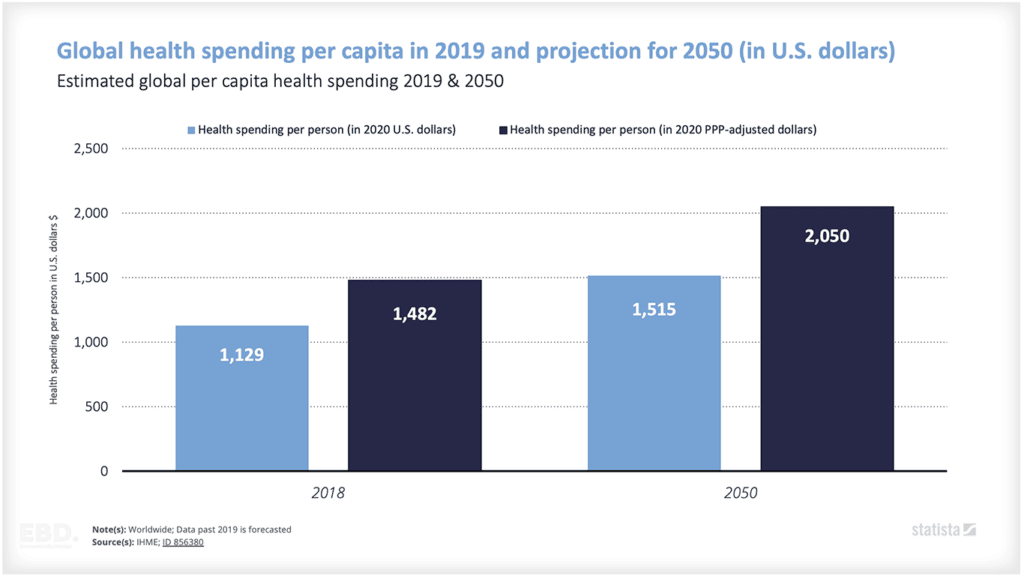
政府资助的医疗服务约占医疗支出的60%。 [1].政府面临的巨大挑战之一是如何在不同地区和不同人群中分享这些资源,以实现当地服务的公平性。
最早的 "公平分享 "公式的例子之一是英国国家医疗服务系统(NHS)用于向区域卫生机构分配资源的公式。最初被称为 "克罗斯曼公式 [2]该方法是由一个成立于1975年的工作小组制定的,被称为资源分配工作小组(RAWP)。
RAWP公式被用来设定目标资金分配,其基础是让那些有同等需求的人有同等机会获得医疗服务。该公式相对粗略,但与之前的历史资金相比,有了巨大的改进,显示出资金方面巨大的不必要的差异,特别是对伦敦的倾斜。
20世纪80年代末,我在财政部工作的早期,曾参与了RAWP的审查工作。这次审查的结果是建立了一个更复杂的公式,此后一直在不断地改进。
随着它的改进,它不再被用来向14个地区分配资金,而是被发展为能够为200多个地方委托团体提供按人头计算的资金方法。尽管进行了几次大的修改,但基本方法至今仍在使用 [3].
配置效率
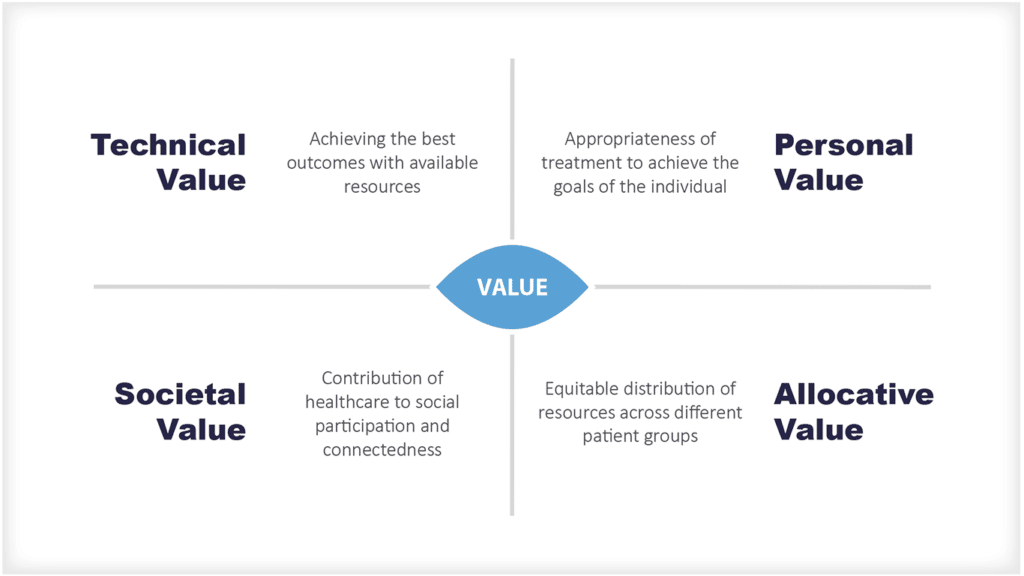
从经济角度看,这就是 "分配效率",即确保医疗服务的基本需求和供应之间的地理一致性 [4].
什么是重要的设计原则?
有几个重要的设计原则影响着这些公式。
- 护理环境(例如,初级保健、医院服务、社区卫生服务、预防等)。
- 资助的服务(例如,产科、精神健康、普通急症服务)。
- 将影响这些服务的决定因素或因素。 需要这些服务的决定因素(例如,人口规模、人口统计学、社会经济学、流行病学等)。
- 影响这些服务的决定性因素有 供应这些服务的决定因素(例如,历史上的服务提供、当地的操作政策(预防与治疗/反应)、部门间的利益相关者关系(很少有公共服务是在真空中提供的),以及替代性的提供(例如私营部门)。
- 供应对感知的服务需求的影响(例如,对于那些将业务政策重点放在预防上的地方,这可能会减少案件数量,这将被视为需求减少的证据--然而潜在的需求可能根本没有改变)。
- 不可避免的费用差异(例如,特别是由于当地劳动力市场条件)。
- 政府对这些服务的战略政策目标,以及是否需要对某些做法进行激励或劝阻。这方面的一个很好的例子是目前NHS对减少手术等待名单的优先考虑。
- 为保持公式的及时性、频率和准确性而提供的数据的及时性。
- 公式的清晰度和透明度以及对 "公平份额 "的看法。
- 地方一级的目标分配与当前的分配,与目标的距离。
- 随着数据的逐年更新,目标分配的稳定性。
- 涵盖从当前到目标分配的变化速度的政策。
这需要考虑的问题相当多。因此,对于什么应该被包括和排除,使用什么数据,以及如何确保公式的真正公平,总是有一个健康的方法论辩论,这并不令人惊讶。这也不奇怪,有一支卫生经济学家大军为这一挑战奉献了他们的职业生涯。
纵横捭阖VS纵横捭阖
公平份额公式的最大挑战之一是,你需要把钱从一个地区(损失地区)转移到另一个地区(收益地区)。从政治和政策的角度来看,这是很棘手的。
即使失去的地区需求相对较低,但以前资源丰富,而获得的地区需求相对较高,但历史上资源水平较低,这也很棘手。然而,如果一个高需求的地区也是一个失败者,那就更难了。
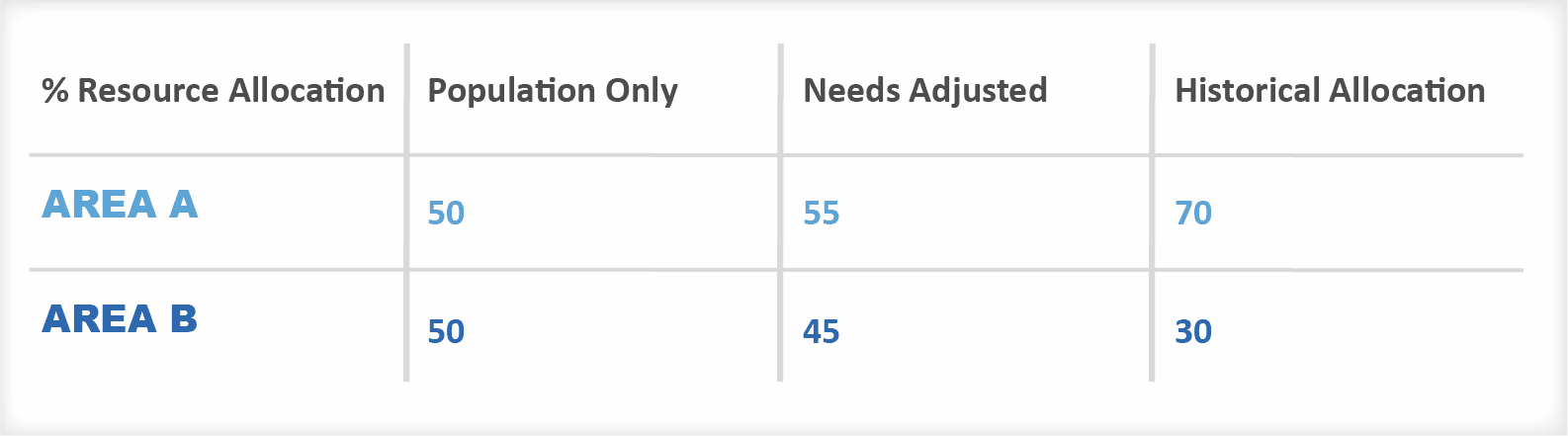
想一想A区与B区的对比--就人口而言,两者规模相同。如果我们假设A区的需求比B区多10%,那么根据需求进行分配,A区将获得55%的可用资金。
但是,如果地区A在历史上获得了70%的资金。分配效率表明,我们应该把钱从A区转移到B区,即使B区的需求较少。
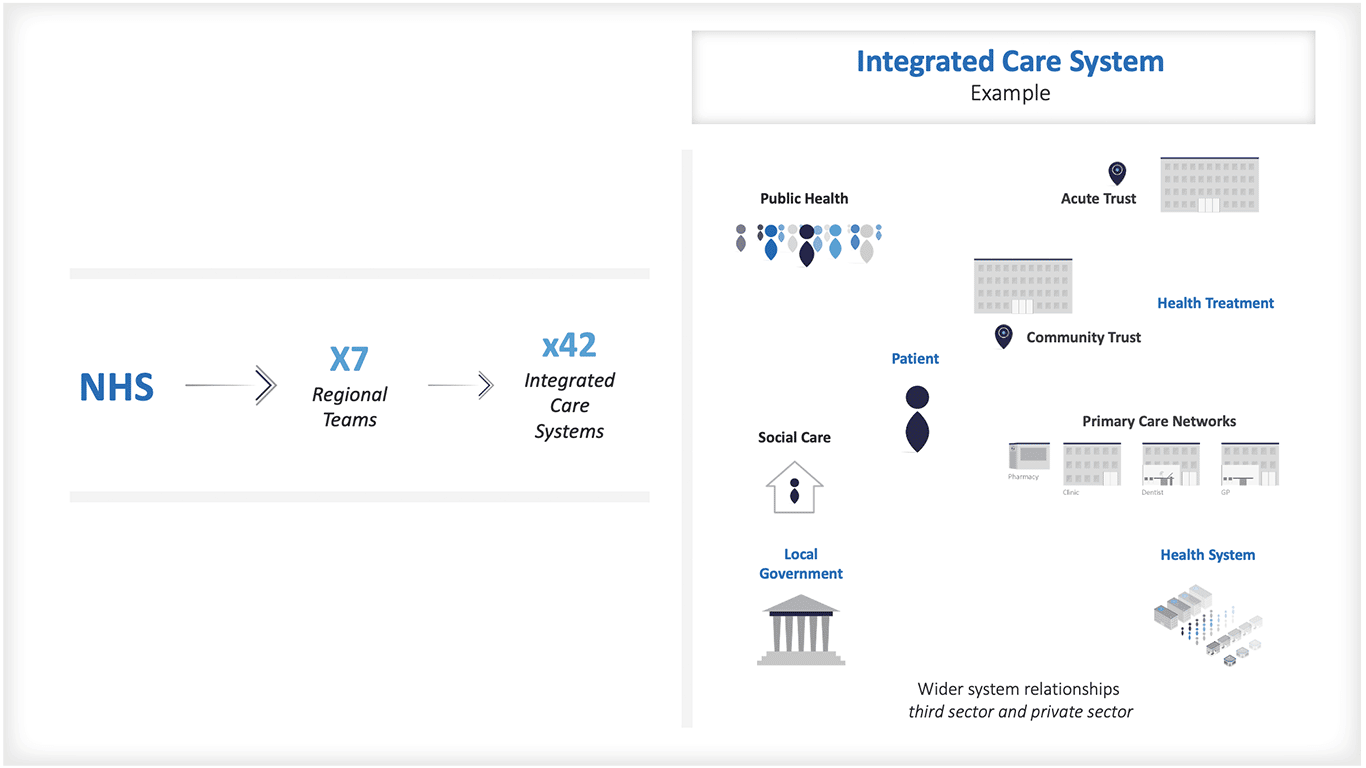
综合护理系统很可能必须平衡战略采购、能力发展以及改善人口健康和减少健康不平等的目标举措。也许公平分配资金的公式方法在未来将被限制在区域分配上?
[1] https://www.economicsbydesign.com/the-economics-of-health-financing-how-much-is-enough/
[2] https://www.kingsfund.org.uk/sites/default/files/field/field_publication_file/improving-the-allocation-of-health-resources-in-england-kingsfund-apr13.pdf
[3] https://www.england.nhs.uk/publication/infographics-fair-shares-a-guide-to-nhs-allocations/
[4] https://www.economicsbydesign.com/economics-and-value-based-healthcare/