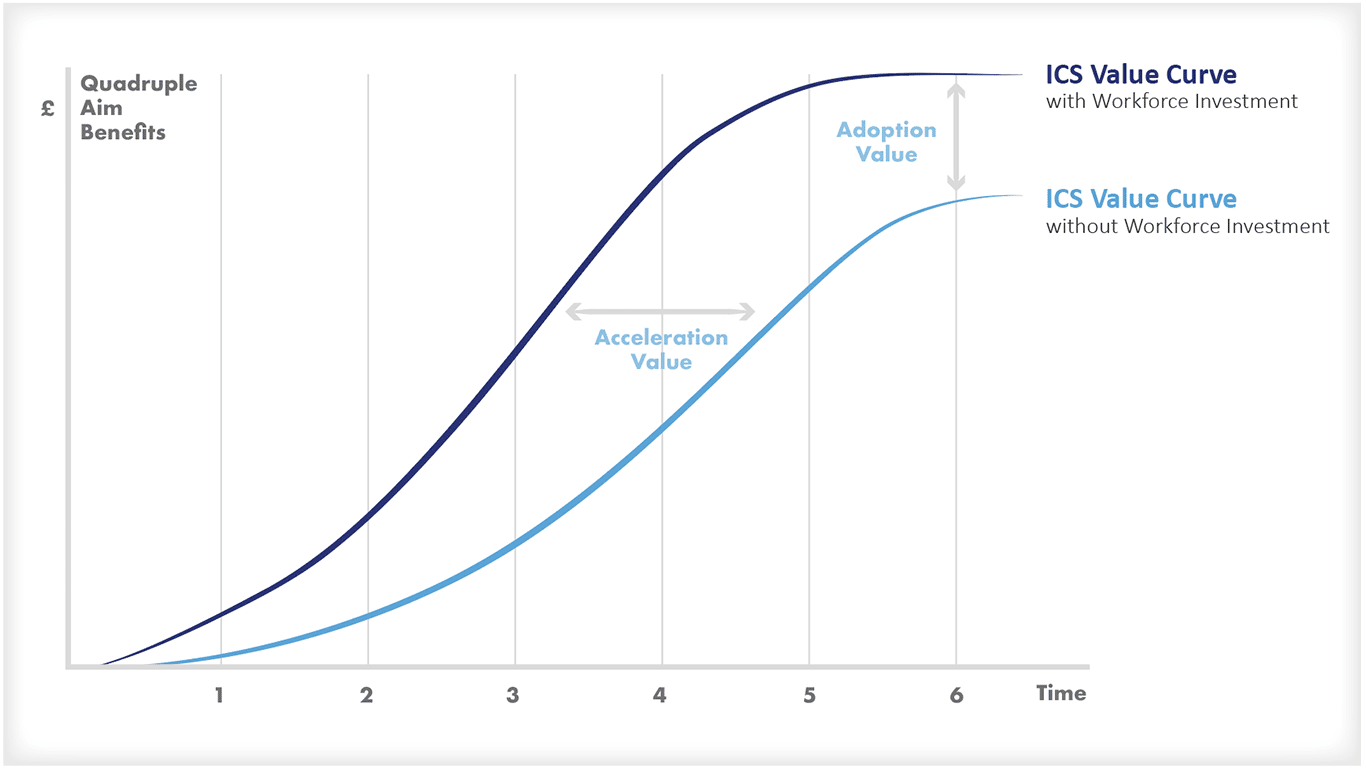
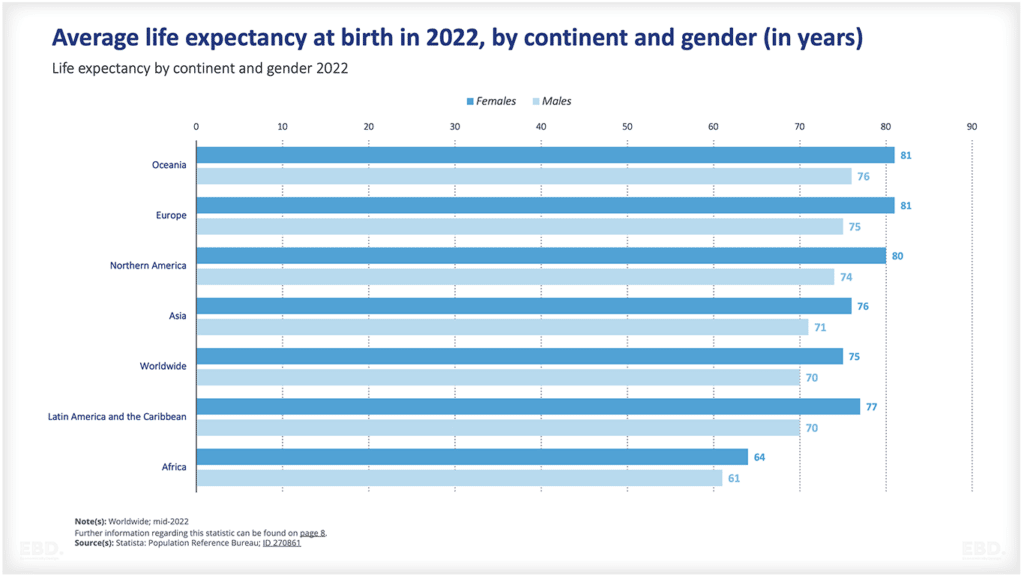
在COVID-19大流行期间,社会价值取决于健康的人口,这一点已经变得非常明显。一个健康的人口是由一支高绩效和多样化的卫生专业人员队伍推动的。
是什么推动了保健和护理专业人员的 "市场"?
最简单的是,对医务人员队伍的需求规模以及技能、经验和专业知识的相对组合是由基本的人口健康、治疗和护理需求、健康和护理模式、健康和护理系统设计和资金驱动的。
保健和护理人员供应的规模和多样性由教育和培训、就业的经济和非经济回报以及这些与其他职业选择的比较所驱动。
当然,事情并没有那么简单。
- 有超过350种不同的健康和护理专业职业[1].每种职业都有不同的需求和供应驱动因素。
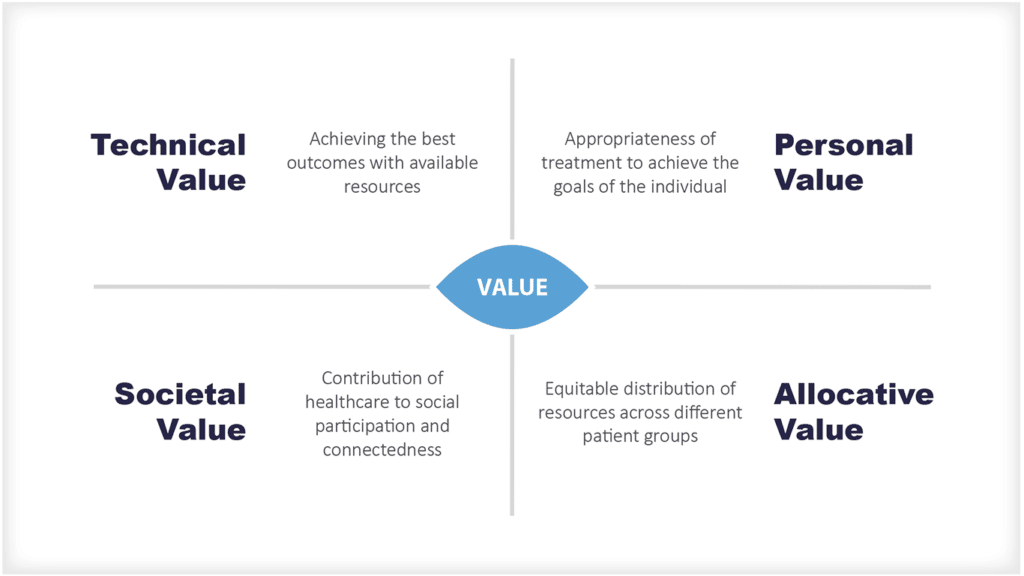
- 健康和护理专业人员不是孤立地工作,他们在护理环境、护理路径和地理网络中组合成多专业、多学科的团队,并利用药物、设备和其他技术及物理基础设施来提供服务。衡量价值时,背景很重要。
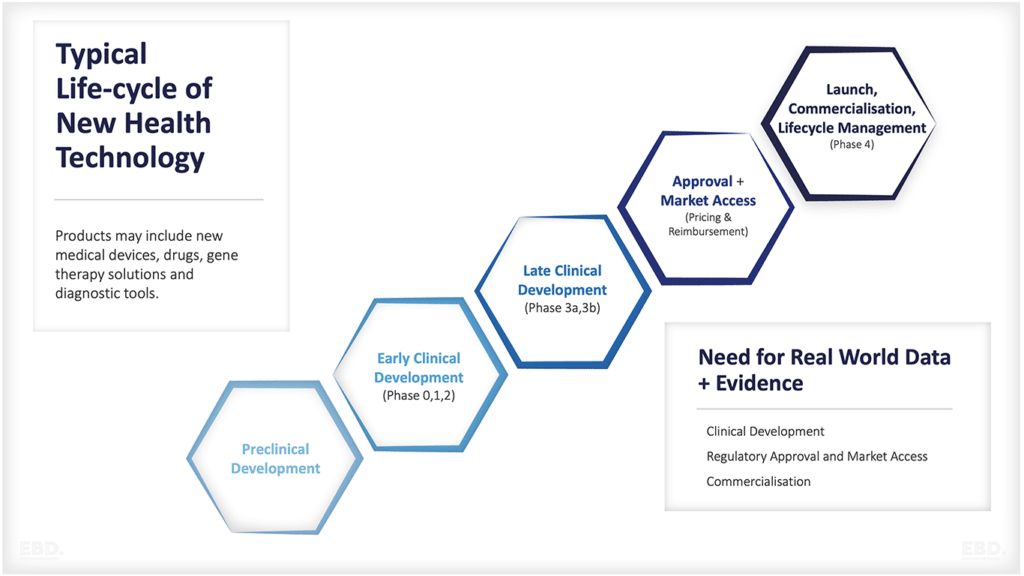
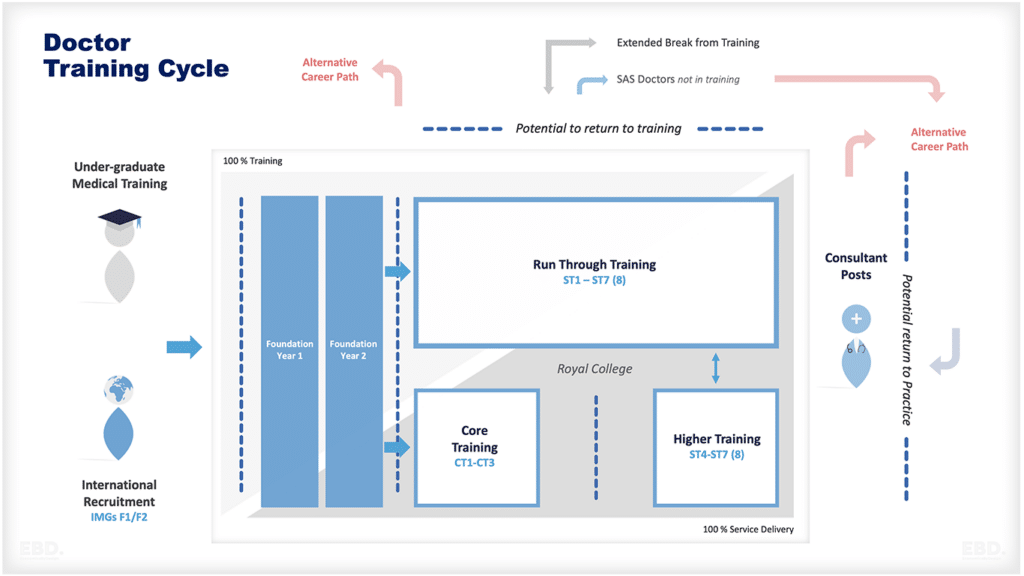
- 根据不同的角色,可能需要多年的培训才能达到职业目标。培训对个人和雇主来说都很昂贵。据PSSRU估计,培训一名NHS顾问的成本超过50万英镑。[2]毕业生和研究生培训至少需要12-13年的时间。更加复杂的是,有很多资金流来支持受训者和雇主支付这些费用,而且这些资金流在各行业中并不一致。
- 在NHS中,薪酬水平通常是由国家规定的。鉴于一些学科和服务领域的长期空缺水平,以及关键专业群体相对较多地使用机构或临时人员,这些水平可能在一定程度上低于这一资源的真正市场价格。[3].
- 在全球范围内,卫生专业人员长期短缺--预测表明,到2030年,主要在中低收入国家将出现1800万的短缺。发达国家在帮助解决这一短缺方面可以发挥作用,而不仅仅是依靠海外工作人员来填补当地供应的缺口。
是什么推动了健康和护理专业人员的价值?
对于一个综合护理系统(ICS)来说,为了从投资中获得最大的价值,关于如何最好地利用卫生和护理人员的价值的考虑必须在议程上占据非常重要的位置。劳动力规划不仅仅是为了获得正确的数字[4]它也是关于卫生经济学的。从劳动力的发展和支持中获得最大的投资回报是至关重要的。
在ICS内有许多雇主可以投资的策略。
增加供应
(例如:留住人才的策略和鼓励重返工作岗位的策略)
发展技能
(例如,高等和研究生培训)
部署新的工作方式
(例如多专业团队)
利用新角色
(例如,通过推进实践)
提高领导力
(影响到组织设计、文化、奖励和激励、员工士气、工作经验)[5]。
所有这些战略都涉及到资源的投资,如时间和技术。所有这些都可以用它们对健康(和护理)系统和更广泛的社会所增加的短期和长期经济价值来衡量。所有这些都需要投资资金,其中一些需要由综合服务中心来协调或支持,而不是由个别的提供者组织。这需要成为劳动力发展计划的组成部分。
让我们开始将卫生经济学纳入劳动力规划,并展示发展和支持劳动力的投资回报,以利于员工、患者和卫生保健系统。
[1] https://www.healthcareers.nhs.uk/explore-roles
[2] https://www.pssru.ac.uk/pub/uc/uc2020/5-sourcesofinfo.pdf
[3] https://nhsfunding.info/symptoms/10-effects-of-underfunding/staff-shortages/
[4]Lewry, C. et al "The Bumper Book of Health and Care Workforce Planning", 2021.
[5] https://heestar.e-lfh.org.uk
请注意。
这是Jacque Mallender的博客的节选版,最初由Tricordant在2022年1月进行了报道。







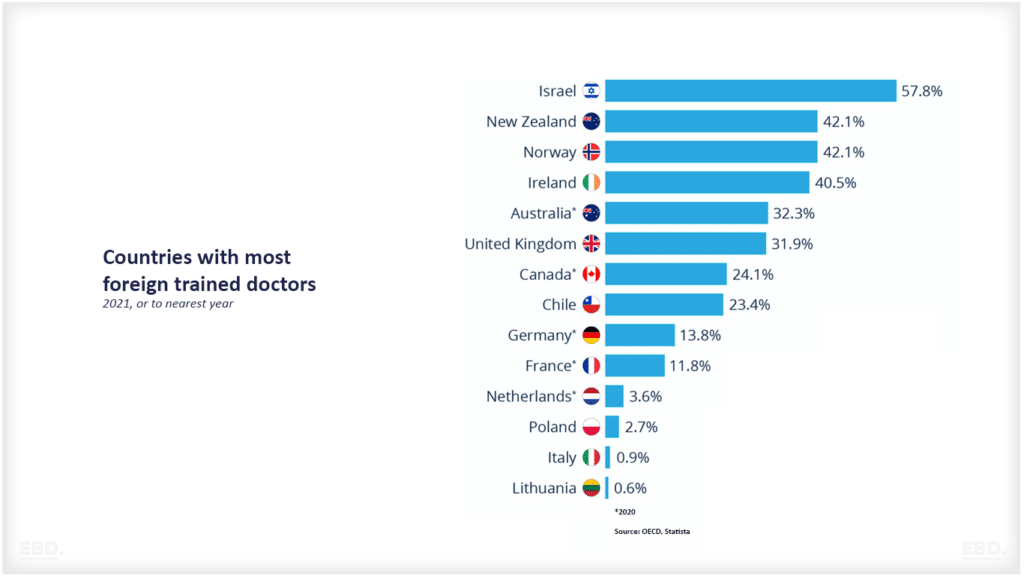






伟大的Jacx,我们需要考虑的一个重要问题是劳动力市场的不平衡,特别是当它涉及到发达国家和欠发达国家之间时,保留战略不能有效地减少差距,或者增加供应可能超出解决差距的能力,人力资源部门是提供综合服务的关键因素,你已经强调了非常重要的问题,需要更多的讨论和想法来解决。
亲爱的Moh
非常感谢您的评论。你强调发达国家和不发达国家之间的不平衡是完全正确的。当发达国家主动吸引不发达国家的工作人员来解决他们自己的短缺问题时,情况就更糟糕了。我们绝对需要围绕这一切进行更多的讨论。也许数字健康可以发挥作用?