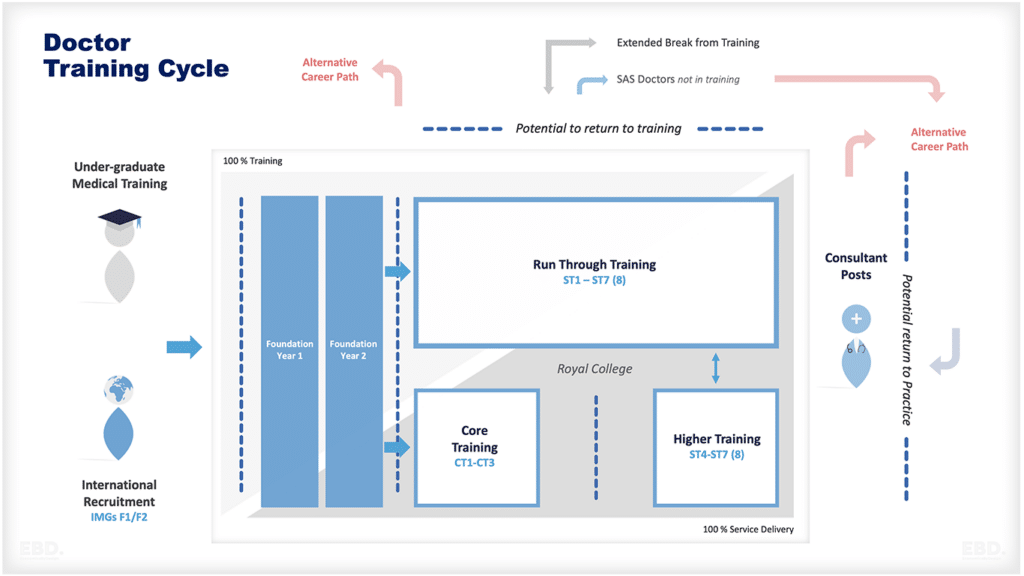
हेल्थकेयर प्रदाताओं के प्रकार
व्यक्ति या आबादी की ओर से स्वास्थ्य सेवाओं को खरीदने के लिए जिम्मेदार लोग (जैसे सार्वजनिक या निजी स्वास्थ्य बीमा कंपनियां या सरकारी क्रय एजेंसियां) एक स्वास्थ्य सेवा प्रदाता के साथ अनुबंध करेंगे।
एक स्वास्थ्य सेवा प्रदाता कोई भी व्यक्ति या संगठन हो सकता है जो स्वास्थ्य सेवाएं प्रदान करता है।
विभिन्न प्रकार के स्वास्थ्य सेवा प्रदाताओं को दो व्यापक समूहों में वर्गीकृत किया जा सकता है:
व्यक्तिगत चिकित्सक:
ये स्वास्थ्य पेशेवर हैं जो स्व-नियोजित हैं और स्वतंत्र रूप से काम करते हैं। उदाहरणों में जीपी, सलाहकार, दंत चिकित्सक, ऑप्टोमेट्रिस्ट और फार्मासिस्ट शामिल हैं।
प्रदाता संगठन:
ये ऐसे संगठन हैं जो स्वास्थ्य देखभाल पेशेवरों के साथ रोजगार या अनुबंध करते हैं और स्वास्थ्य सेवाएं प्रदान करते हैं। उदाहरणों में अस्पताल, जीपी प्रथाएं, सामुदायिक फार्मेसियों और दंत चिकित्सा सर्जरी शामिल हैं।
यह लेख स्वास्थ्य सेवा प्रदाताओं की विभिन्न स्वामित्व संरचनाओं, विभिन्न प्रकार के स्वास्थ्य सेवा प्रदाताओं के उदाहरणों और समेकन और एकीकरण के लिए प्रमुख रुझानों को देखता है।
हेल्थकेयर प्रदाताओं का मालिक कौन है?
विभिन्न प्रकार के स्वास्थ्य सेवा प्रदाता संगठनों के लिए कई स्वामित्व मॉडल हैं। तीन सबसे आम स्वामित्व मॉडल हैं:
सार्वजनिक क्षेत्र के प्रदाता:
ये प्रदाता हैं जो सरकार के स्वामित्व और संचालन में हैं।
निजी क्षेत्र "लाभ के लिए" प्रदाता:
ये प्रदाता हैं जो लाभकारी कंपनियों के स्वामित्व और संचालन में हैं।
निजी क्षेत्र "गैर-लाभकारी" प्रदाता:
ये ऐसे प्रदाता हैं जो निजी स्वामित्व और संचालित होते हैं लेकिन गैर-लाभकारी आधार पर।
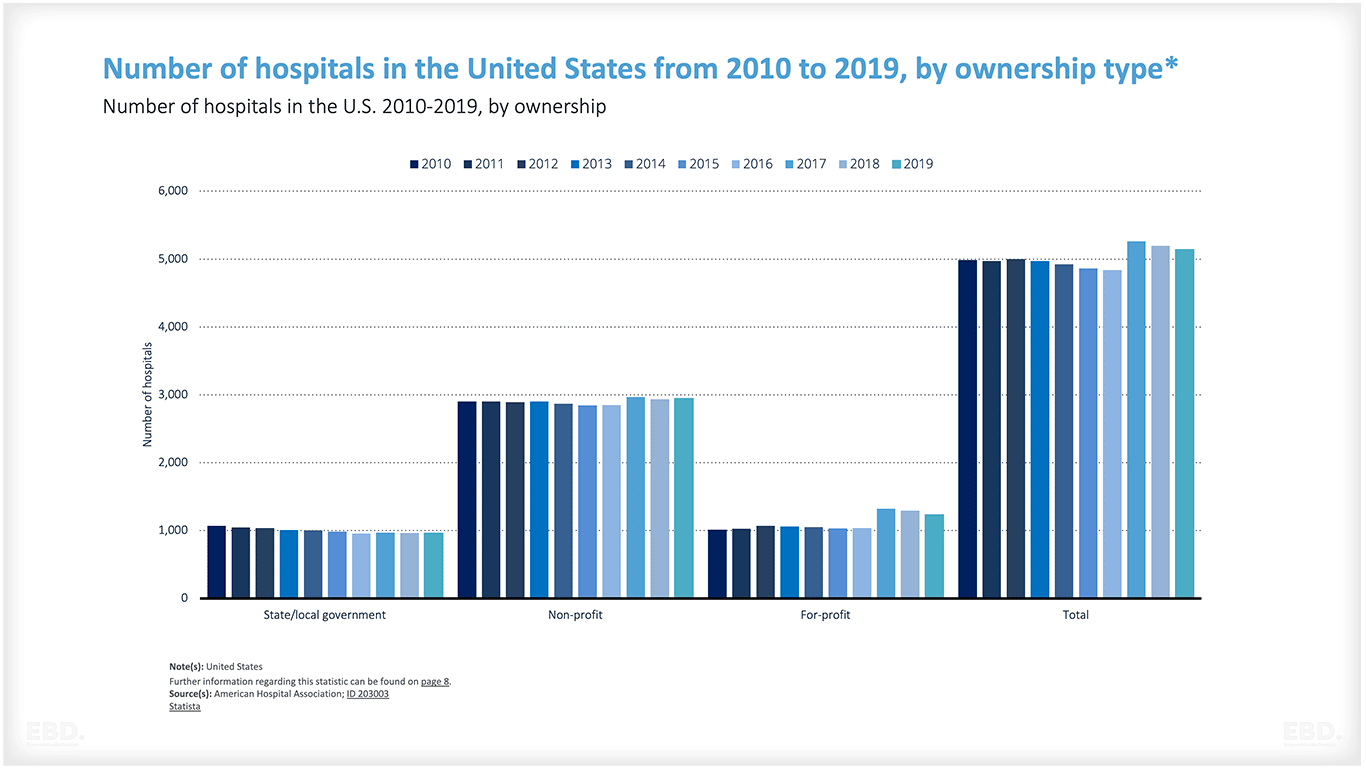
अधिकांश स्वास्थ्य प्रणालियों में देखभाल के सभी स्तरों पर सभी तीन ऑपरेटिंग का मिश्रण होता है।
सार्वजनिक रूप से स्वामित्व वाले प्रदाता
ओईसीडी सार्वजनिक रूप से स्वामित्व वाले अस्पतालों को "अस्पतालों के रूप में परिभाषित करता है जो सरकारी इकाई या किसी अन्य सार्वजनिक निगम के स्वामित्व या नियंत्रण में हैं (जहां नियंत्रण को सामान्य कॉर्पोरेट नीति निर्धारित करने की क्षमता के रूप में परिभाषित किया गया है)" ओईसीडी स्वास्थ्य सांख्यिकी 2022।
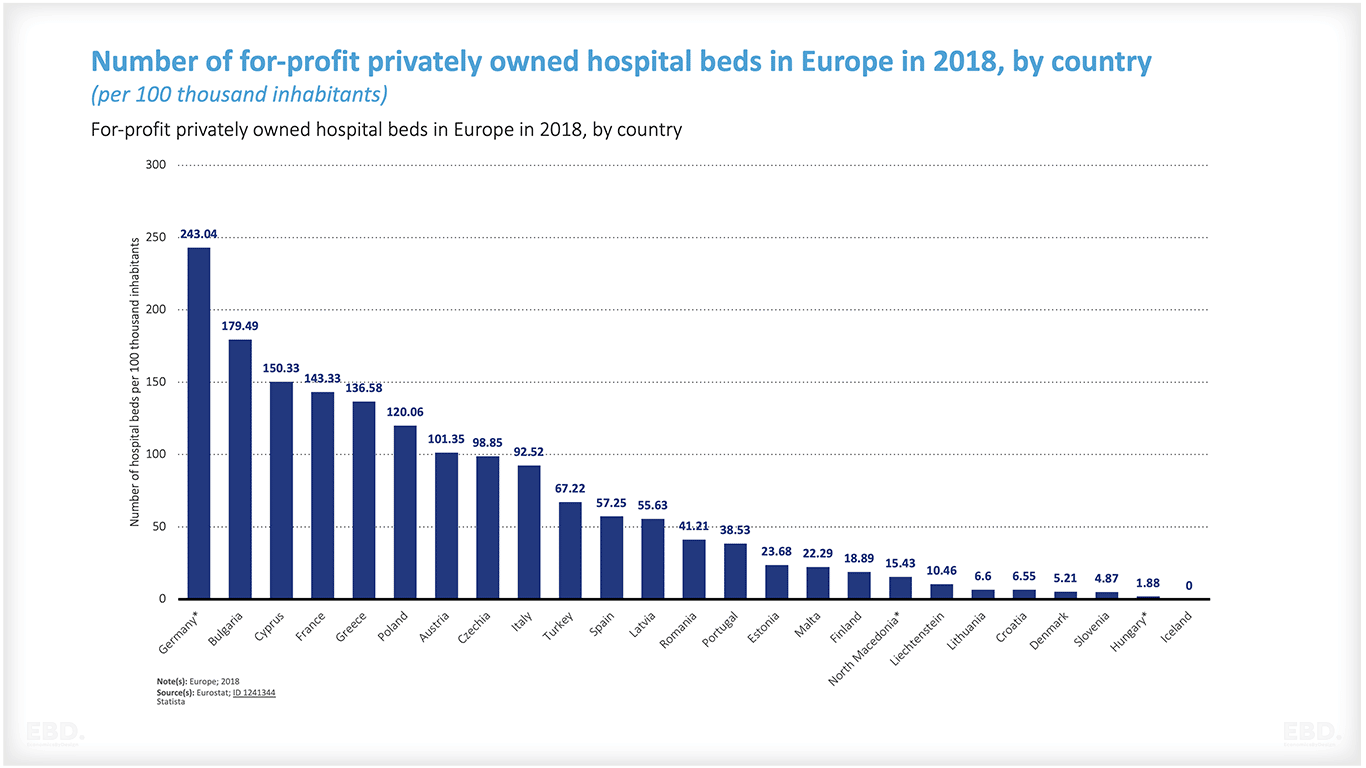
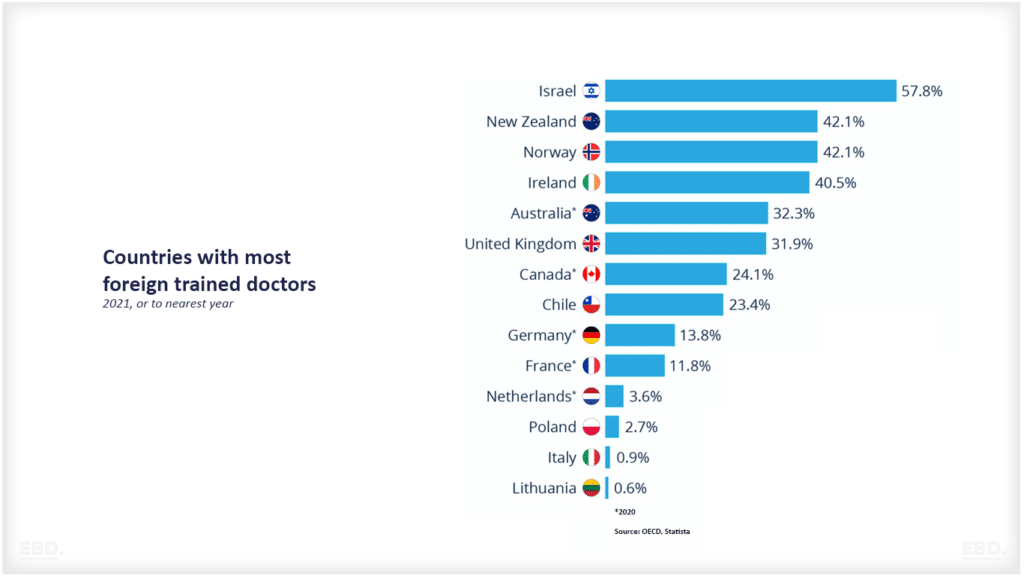
ब्रिटेन में ओईसीडी में सार्वजनिक स्वामित्व वाले अस्पतालों की संख्या सबसे अधिक है, नीदरलैंड के पास सार्वजनिक स्वामित्व में कोई अस्पताल नहीं है।
यूके में, अस्पतालों का स्वामित्व या तो राष्ट्रीय स्वास्थ्य सेवा (एनएचएस) या स्थानीय अधिकारियों के पास है। इंग्लैंड में एनएचएस में, लगभग 240 अस्पताल हैं जो एनएचएस फाउंडेशन ट्रस्ट के स्वामित्व में हैं।
एनएचएस फाउंडेशन ट्रस्ट सार्वजनिक क्षेत्र के संगठन हैं जो निजी कंपनियों के समान तरीके से काम करते हैं। उन्हें अन्य एनएचएस संगठनों की तुलना में यह तय करने की अधिक स्वतंत्रता है कि वे सेवाओं को कैसे व्यवस्थित और वितरित करते हैं। हालांकि, उन्हें अभी भी एनएचएस नियमों का पालन करने की आवश्यकता है।
एक और उदाहरण नीदरलैंड है जहां सभी अस्पताल निजी हैं लेकिन शेयरधारकों (मालिकों) को धन वितरित करने की अनुमति नहीं है और इसलिए अनिवार्य रूप से गैर-लाभकारी प्रदाताओं के रूप में काम करते हैं।
सार्वजनिक रूप से स्वामित्व वाले प्रदाताओं के कई फायदे और नुकसान हैं। कुछ कथित फायदों में शामिल हैं:
- वे आमतौर पर उपयोग के बिंदु पर मुफ्त में काम करते हैं जो देखभाल तक पहुंच बढ़ा सकते हैं।
- वे सरकार के प्रति जवाबदेह हैं जो पारदर्शिता और गुणवत्ता में सुधार कर सकती है।
- वे सरकारी नीति में बदलाव के प्रति अधिक उत्तरदायी हो सकते हैं।
कुछ कथित नुकसानों में शामिल हैं:
- वे उपभोक्ता मांग में बदलाव के लिए कम उत्तरदायी हो सकते हैं।
- प्रतिस्पर्धा के निचले स्तर के कारण वे निजी प्रदाताओं की तुलना में कम कुशल हो सकते हैं।
- वे निजी प्रदाताओं की तुलना में कम अभिनव हो सकते हैं।
निजी क्षेत्र "लाभ के लिए" प्रदाता
ओईसीडी में, निजी स्वामित्व वाले "लाभकारी" अस्पतालों को "अस्पतालों के रूप में परिभाषित किया गया है जो माल और सेवाओं के उत्पादन के उद्देश्य से स्थापित कानूनी संस्थाएं हैं और अपने मालिकों के लिए लाभ या अन्य वित्तीय लाभ उत्पन्न करने में सक्षम हैं" (ओईसीडी स्वास्थ्य सांख्यिकी 2022)।
निजी स्वामित्व वाले प्रदाताओं के उदाहरणों में यूके में बूपा और नफील्ड हेल्थ शामिल हैं। अमेरिका में, एचसीए हेल्थकेयर जैसी लाभकारी अस्पताल श्रृंखलाएं हैं। भारत में, सबसे बड़ा निजी स्वास्थ्य सेवा प्रदाता अपोलो हॉस्पिटल्स एंटरप्राइज लिमिटेड है। निजी अस्पतालों के उच्च अनुपात वाले देशों में चिली, कोलंबिया, कोस्टा रिका, मैक्सिको और पेरू शामिल हैं।
प्राथमिक देखभाल सेवाएं कई देशों में निजी क्षेत्र द्वारा प्रदान की जाती हैं। उदाहरण के लिए, यूके में, कई जीपी उन प्रथाओं में काम करते हैं जो निजी कंपनियों के स्वामित्व में हैं। ऑस्ट्रेलिया में, लाभकारी सामान्य प्रथाएं हैं जिन्हें चिकित्सा केंद्रों के रूप में जाना जाता है।
निजी क्षेत्र "लाभ के लिए नहीं" प्रदाता
ओईसीडी में, निजी स्वामित्व वाले "गैर-लाभकारी" अस्पतालों को "माल और सेवाओं के उत्पादन के उद्देश्य से बनाई गई कानूनी या सामाजिक संस्थाओं" के रूप में परिभाषित किया गया है, जिनकी स्थिति उन्हें इकाई (ओं) के लिए आय, लाभ या अन्य वित्तीय लाभ का स्रोत होने की अनुमति नहीं देती है जो उन्हें स्थापित, नियंत्रित या वित्त पोषित करती है"। (ओईसीडी स्वास्थ्य सांख्यिकी 2022)।
निजी स्वामित्व वाले गैर-लाभकारी अस्पतालों को अक्सर दान या सामाजिक उद्यमों के रूप में स्थापित किया जाता है। ओईसीडी के आंकड़ों (2020) के अनुसार, कोरिया में प्रति मिलियन आबादी पर गैर-लाभकारी अस्पतालों की उच्चतम रिपोर्ट दर है। संयुक्त राज्य अमेरिका के कुछ सबसे प्रसिद्ध अस्पताल गैर-लाभकारी हैं और इसमें मेयो क्लिनिक, क्लीवलैंड क्लिनिक और जॉन्स हॉपकिंस शामिल हैं।
सिर्फ इसलिए कि एक प्रदाता को "लाभ के लिए नहीं" के रूप में वर्णित किया गया है, इसका मतलब यह नहीं है कि वे लाभदायक नहीं हैं। स्वास्थ्य मामलों में एक अपेक्षाकृत हालिया अध्ययन से पता चला है कि रोगी सेवाओं से उच्चतम लाभ वाले शीर्ष 10 अस्पतालों में से 7 "गैर-लाभकारी" थे।
स्वास्थ्य सेवा प्रदाताओं को कैसे व्यवस्थित किया जाता है?
स्वास्थ्य सेवा प्रदाताओं को कैसे व्यवस्थित किया जा सकता है, इसके लिए कई अलग-अलग मॉडल हैं।
अस्पताल स्टैंडअलोन संगठन हो सकते हैं या वे एक बड़ी प्रणाली का हिस्सा हो सकते हैं। उदाहरण के लिए, यूके में, अधिकांश अस्पताल एनएचएस फाउंडेशन ट्रस्ट के स्वामित्व में हैं जो एनएचएस से अलग कानूनी संस्थाएं हैं। अमेरिका में, अस्पताल एक अस्पताल प्रणाली का हिस्सा हो सकते हैं जो एक ही संगठन के स्वामित्व वाले कई अस्पतालों का संग्रह है।
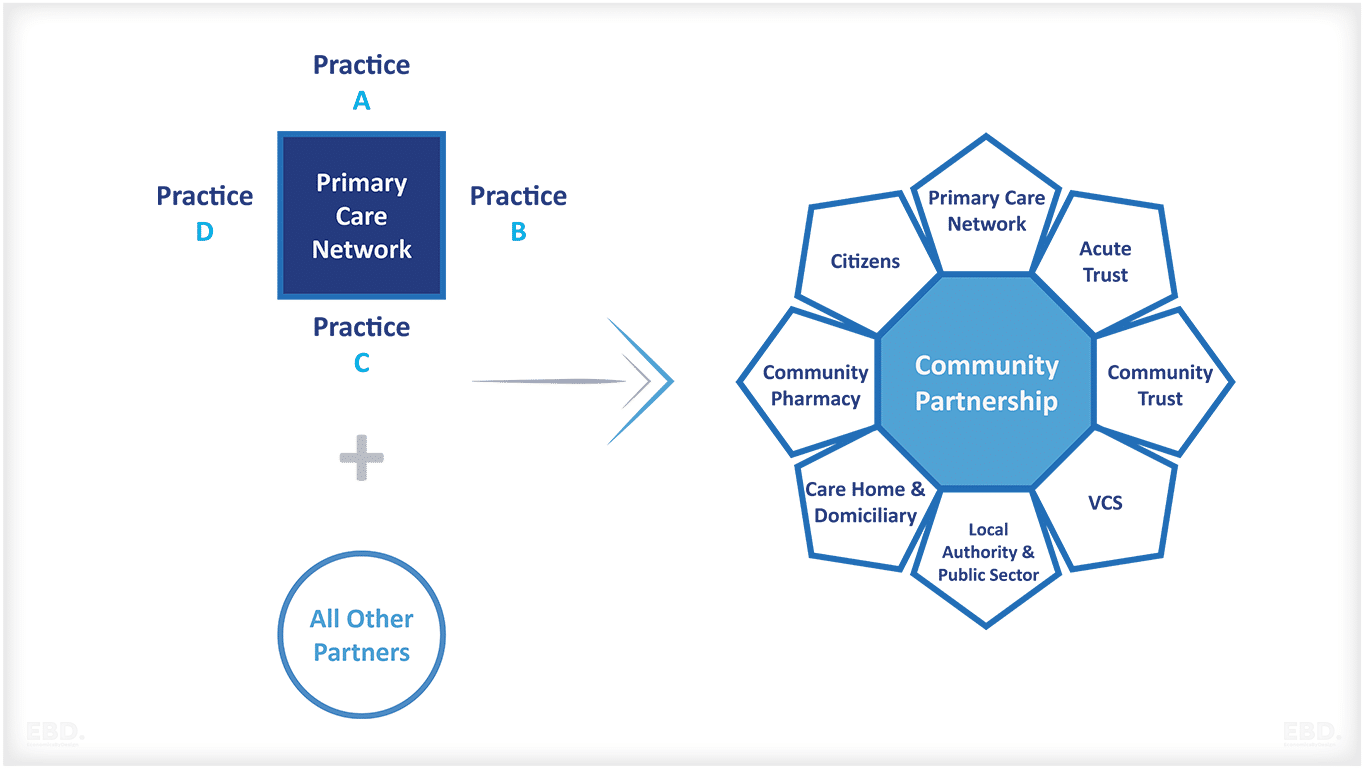
प्राथमिक देखभाल प्रदाता स्टैंडअलोन संगठन भी हो सकते हैं या वे प्राथमिक देखभाल नेटवर्क (पीसीएन) का हिस्सा हो सकते हैं। पीसीएन सामान्य प्रथाओं के समूह हैं जो अपने रोगियों के लिए एकीकृत देखभाल प्रदान करने के लिए एक साथ काम करते हैं (एनएचएस इंग्लैंड, 2020)।
कुछ देशों में, प्रदाताओं को "प्रदाता समूहों" में व्यवस्थित किया जाता है। इन्हें "स्वायत्त, बहु-पेशेवर संगठनों के रूप में परिभाषित किया गया है जो आबादी की स्वास्थ्य आवश्यकताओं के लिए जिम्मेदार और जवाबदेह हैं" (ओईसीडी, 2016)। प्रदाता समूह सार्वजनिक, निजी या दोनों का मिश्रण हो सकते हैं।
विभिन्न प्रकार के स्वास्थ्य सेवा प्रदाता क्या हैं?
स्वास्थ्य सेवा संगठनों में उन सेवाओं (क्षैतिज एकीकरण) और देखभाल के स्तर (ऊर्ध्वाधर एकीकरण) में एकीकरण की डिग्री के संदर्भ में भारी विविधता है। यहाँ सबसे आम में से कुछ हैं:
जवाबदेह देखभाल संगठन
एक जवाबदेह देखभाल संगठन (एसीओ) एक प्रकार का प्रदाता समूह है जो अमेरिका में आम है। एसीओ "डॉक्टरों, अस्पतालों और अन्य स्वास्थ्य देखभाल प्रदाताओं के समूह हैं जो अपने मेडिकेयर रोगियों को समन्वित उच्च गुणवत्ता वाली देखभाल देने के लिए स्वेच्छा से एक साथ आते हैं" (मेडिकेयर और मेडिकेड सर्विसेज, 2020 के लिए केंद्र)।
एकीकृत वितरण नेटवर्क
एक एकीकृत वितरण नेटवर्क (आईडीएन) एक अन्य प्रकार का प्रदाता समूह है जो अमेरिका में आम है। आईडीएन "अस्पतालों, चिकित्सकों और अन्य प्रदाताओं के समूह हैं जो समन्वित, उच्च गुणवत्ता वाली देखभाल प्रदान करने के लिए बलों में शामिल हो गए हैं" (अमेरिकन हॉस्पिटल एसोसिएशन, 2020)। आईडीएन सार्वजनिक, निजी या दोनों का मिश्रण हो सकता है। अमेरिका में सबसे बड़े आईडीएन में से एक पार्टनर्स हेल्थकेयर है जो एक निजी गैर-लाभकारी संगठन है।
एम्बुलेटरी सर्जिकल सेंटर
एम्बुलेटरी सर्जिकल सेंटर (एएससी) एक प्रकार का प्रदाता है जो आउट पेशेंट सर्जरी में माहिर है। एएससी आमतौर पर अमेरिका में पाए जाते हैं और वे या तो लाभ के लिए या गैर-लाभकारी हो सकते हैं।
चिकित्सक-अस्पताल संगठन
एक चिकित्सक-अस्पताल संगठन (पीएचओ) एक प्रकार का प्रदाता समूह है जो अमेरिका में आम है। पीएचओ "एक या एक से अधिक अस्पतालों और चिकित्सकों के एक समूह से मिलकर संगठन हैं जो देखभाल की गुणवत्ता और दक्षता में सुधार के लिए बलों में शामिल हो गए हैं" (अमेरिकन हॉस्पिटल एसोसिएशन, 2020)।
पीएचओ सार्वजनिक, निजी या दोनों का मिश्रण हो सकता है। अमेरिका में सबसे बड़े पीएचओ में से एक मेयो क्लिनिक है जो एक निजी गैर-लाभकारी संगठन है।
रोगी-केंद्रित चिकित्सा गृह
एक रोगी केंद्रित चिकित्सा घर (पीसीएमएच) एक प्रकार का प्राथमिक देखभाल मॉडल है जो अमेरिका में सस्ती देखभाल अधिनियम (2010) के बाद से आम है और दुनिया भर में तेजी से आम है। पीसीएमएच की मुख्य विशेषताएं हैं:
- देखभाल के लिए एक टीम-आधारित दृष्टिकोण
- एक संपूर्ण व्यक्ति फोकस
- व्यापक देखभाल
- समन्वित देखभाल
- सुलभ देखभाल
प्राथमिक देखभाल नेटवर्क
एक प्राथमिक देखभाल नेटवर्क (पीसीएन) एक प्रकार का प्रदाता समूह है जो यूके में आम है। पीसीएन "सामान्य प्रथाओं के समूह हैं जो अपने रोगियों के लिए एकीकृत देखभाल प्रदान करने के लिए एक साथ काम करते हैं" (एनएचएस इंग्लैंड, 2020)।
ब्रिटेन में ओईसीडी में सार्वजनिक स्वामित्व वाले अस्पतालों की संख्या सबसे अधिक है, नीदरलैंड के पास सार्वजनिक स्वामित्व में कोई अस्पताल नहीं है।
यूके में, अस्पतालों का स्वामित्व या तो राष्ट्रीय स्वास्थ्य सेवा (एनएचएस) या स्थानीय अधिकारियों के पास है। इंग्लैंड में एनएचएस में, लगभग 240 अस्पताल हैं जो एनएचएस फाउंडेशन ट्रस्ट के स्वामित्व में हैं।
एनएचएस फाउंडेशन ट्रस्ट सार्वजनिक क्षेत्र के संगठन हैं जो निजी कंपनियों के समान तरीके से काम करते हैं। उन्हें अन्य एनएचएस संगठनों की तुलना में यह तय करने की अधिक स्वतंत्रता है कि वे सेवाओं को कैसे व्यवस्थित और वितरित करते हैं। हालांकि, उन्हें अभी भी एनएचएस नियमों का पालन करने की आवश्यकता है।
एक और उदाहरण नीदरलैंड है जहां सभी अस्पताल निजी हैं लेकिन शेयरधारकों (मालिकों) को धन वितरित करने की अनुमति नहीं है और इसलिए अनिवार्य रूप से गैर-लाभकारी प्रदाताओं के रूप में काम करते हैं।
सार्वजनिक रूप से स्वामित्व वाले प्रदाताओं के कई फायदे और नुकसान हैं। कुछ कथित फायदों में शामिल हैं:
- वे आमतौर पर उपयोग के बिंदु पर मुफ्त में काम करते हैं जो देखभाल तक पहुंच बढ़ा सकते हैं।
- वे सरकार के प्रति जवाबदेह हैं जो पारदर्शिता और गुणवत्ता में सुधार कर सकती है।
- वे सरकारी नीति में बदलाव के प्रति अधिक उत्तरदायी हो सकते हैं।
कुछ कथित नुकसानों में शामिल हैं:
- वे उपभोक्ता मांग में बदलाव के लिए कम उत्तरदायी हो सकते हैं।
- प्रतिस्पर्धा के निचले स्तर के कारण वे निजी प्रदाताओं की तुलना में कम कुशल हो सकते हैं।
- वे निजी प्रदाताओं की तुलना में कम अभिनव हो सकते हैं।
निजी क्षेत्र "लाभ के लिए" प्रदाता
ओईसीडी में, निजी स्वामित्व वाले "लाभकारी" अस्पतालों को "अस्पतालों के रूप में परिभाषित किया गया है जो माल और सेवाओं के उत्पादन के उद्देश्य से स्थापित कानूनी संस्थाएं हैं और अपने मालिकों के लिए लाभ या अन्य वित्तीय लाभ उत्पन्न करने में सक्षम हैं" (ओईसीडी स्वास्थ्य सांख्यिकी 2022)।
निजी स्वामित्व वाले प्रदाताओं के उदाहरणों में यूके में बूपा और नफील्ड हेल्थ शामिल हैं। अमेरिका में, एचसीए हेल्थकेयर जैसी लाभकारी अस्पताल श्रृंखलाएं हैं। भारत में, सबसे बड़ा निजी स्वास्थ्य सेवा प्रदाता अपोलो हॉस्पिटल्स एंटरप्राइज लिमिटेड है। निजी अस्पतालों के उच्च अनुपात वाले देशों में चिली, कोलंबिया, कोस्टा रिका, मैक्सिको और पेरू शामिल हैं।
प्राथमिक देखभाल सेवाएं कई देशों में निजी क्षेत्र द्वारा प्रदान की जाती हैं। उदाहरण के लिए, यूके में, कई जीपी उन प्रथाओं में काम करते हैं जो निजी कंपनियों के स्वामित्व में हैं। ऑस्ट्रेलिया में, लाभकारी सामान्य प्रथाएं हैं जिन्हें चिकित्सा केंद्रों के रूप में जाना जाता है।
निजी क्षेत्र "लाभ के लिए नहीं" प्रदाता
ओईसीडी में, निजी स्वामित्व वाले "गैर-लाभकारी" अस्पतालों को "माल और सेवाओं के उत्पादन के उद्देश्य से बनाई गई कानूनी या सामाजिक संस्थाओं" के रूप में परिभाषित किया गया है, जिनकी स्थिति उन्हें इकाई (ओं) के लिए आय, लाभ या अन्य वित्तीय लाभ का स्रोत होने की अनुमति नहीं देती है जो उन्हें स्थापित, नियंत्रित या वित्त पोषित करती है"। (ओईसीडी स्वास्थ्य सांख्यिकी 2022)।
निजी स्वामित्व वाले गैर-लाभकारी अस्पतालों को अक्सर दान या सामाजिक उद्यमों के रूप में स्थापित किया जाता है। ओईसीडी के आंकड़ों (2020) के अनुसार, कोरिया में प्रति मिलियन आबादी पर गैर-लाभकारी अस्पतालों की उच्चतम रिपोर्ट दर है। संयुक्त राज्य अमेरिका के कुछ सबसे प्रसिद्ध अस्पताल गैर-लाभकारी हैं और इसमें मेयो क्लिनिक, क्लीवलैंड क्लिनिक और जॉन्स हॉपकिंस शामिल हैं।
सिर्फ इसलिए कि एक प्रदाता को "लाभ के लिए नहीं" के रूप में वर्णित किया गया है, इसका मतलब यह नहीं है कि वे लाभदायक नहीं हैं। स्वास्थ्य मामलों में एक अपेक्षाकृत हालिया अध्ययन से पता चला है कि रोगी सेवाओं से उच्चतम लाभ वाले शीर्ष 10 अस्पतालों में से 7 "गैर-लाभकारी" थे।
स्वास्थ्य सेवा प्रदाताओं को कैसे व्यवस्थित किया जाता है?
स्वास्थ्य सेवा प्रदाताओं को कैसे व्यवस्थित किया जा सकता है, इसके लिए कई अलग-अलग मॉडल हैं।
अस्पताल स्टैंडअलोन संगठन हो सकते हैं या वे एक बड़ी प्रणाली का हिस्सा हो सकते हैं। उदाहरण के लिए, यूके में, अधिकांश अस्पताल एनएचएस फाउंडेशन ट्रस्ट के स्वामित्व में हैं जो एनएचएस से अलग कानूनी संस्थाएं हैं। अमेरिका में, अस्पताल एक अस्पताल प्रणाली का हिस्सा हो सकते हैं जो एक ही संगठन के स्वामित्व वाले कई अस्पतालों का संग्रह है।
प्राथमिक देखभाल प्रदाता स्टैंडअलोन संगठन भी हो सकते हैं या वे प्राथमिक देखभाल नेटवर्क (पीसीएन) का हिस्सा हो सकते हैं। पीसीएन सामान्य प्रथाओं के समूह हैं जो अपने रोगियों के लिए एकीकृत देखभाल प्रदान करने के लिए एक साथ काम करते हैं (एनएचएस इंग्लैंड, 2020)।
कुछ देशों में, प्रदाताओं को "प्रदाता समूहों" में व्यवस्थित किया जाता है। इन्हें "स्वायत्त, बहु-पेशेवर संगठनों के रूप में परिभाषित किया गया है जो आबादी की स्वास्थ्य आवश्यकताओं के लिए जिम्मेदार और जवाबदेह हैं" (ओईसीडी, 2016)। प्रदाता समूह सार्वजनिक, निजी या दोनों का मिश्रण हो सकते हैं।
विभिन्न प्रकार के स्वास्थ्य सेवा प्रदाता क्या हैं?
स्वास्थ्य सेवा संगठनों में उन सेवाओं (क्षैतिज एकीकरण) और देखभाल के स्तर (ऊर्ध्वाधर एकीकरण) में एकीकरण की डिग्री के संदर्भ में भारी विविधता है। यहाँ सबसे आम में से कुछ हैं:
जवाबदेह देखभाल संगठन
एक जवाबदेह देखभाल संगठन (एसीओ) एक प्रकार का प्रदाता समूह है जो अमेरिका में आम है। एसीओ "डॉक्टरों, अस्पतालों और अन्य स्वास्थ्य देखभाल प्रदाताओं के समूह हैं जो अपने मेडिकेयर रोगियों को समन्वित उच्च गुणवत्ता वाली देखभाल देने के लिए स्वेच्छा से एक साथ आते हैं" (मेडिकेयर और मेडिकेड सर्विसेज, 2020 के लिए केंद्र)।
एकीकृत वितरण नेटवर्क
एक एकीकृत वितरण नेटवर्क (आईडीएन) एक अन्य प्रकार का प्रदाता समूह है जो अमेरिका में आम है। आईडीएन "अस्पतालों, चिकित्सकों और अन्य प्रदाताओं के समूह हैं जो समन्वित, उच्च गुणवत्ता वाली देखभाल प्रदान करने के लिए बलों में शामिल हो गए हैं" (अमेरिकन हॉस्पिटल एसोसिएशन, 2020)। आईडीएन सार्वजनिक, निजी या दोनों का मिश्रण हो सकता है। अमेरिका में सबसे बड़े आईडीएन में से एक पार्टनर्स हेल्थकेयर है जो एक निजी गैर-लाभकारी संगठन है।
एम्बुलेटरी सर्जिकल सेंटर
एम्बुलेटरी सर्जिकल सेंटर (एएससी) एक प्रकार का प्रदाता है जो आउट पेशेंट सर्जरी में माहिर है। एएससी आमतौर पर अमेरिका में पाए जाते हैं और वे या तो लाभ के लिए या गैर-लाभकारी हो सकते हैं।
चिकित्सक-अस्पताल संगठन
एक चिकित्सक-अस्पताल संगठन (पीएचओ) एक प्रकार का प्रदाता समूह है जो अमेरिका में आम है। पीएचओ "एक या एक से अधिक अस्पतालों और चिकित्सकों के एक समूह से मिलकर संगठन हैं जो देखभाल की गुणवत्ता और दक्षता में सुधार के लिए बलों में शामिल हो गए हैं" (अमेरिकन हॉस्पिटल एसोसिएशन, 2020)।
पीएचओ सार्वजनिक, निजी या दोनों का मिश्रण हो सकता है। अमेरिका में सबसे बड़े पीएचओ में से एक मेयो क्लिनिक है जो एक निजी गैर-लाभकारी संगठन है।
रोगी-केंद्रित चिकित्सा गृह
एक रोगी केंद्रित चिकित्सा घर (पीसीएमएच) एक प्रकार का प्राथमिक देखभाल मॉडल है जो अमेरिका में सस्ती देखभाल अधिनियम (2010) के बाद से आम है और दुनिया भर में तेजी से आम है। पीसीएमएच की मुख्य विशेषताएं हैं:
- देखभाल के लिए एक टीम-आधारित दृष्टिकोण
- एक संपूर्ण व्यक्ति फोकस
- व्यापक देखभाल
- समन्वित देखभाल
- सुलभ देखभाल
प्राथमिक देखभाल नेटवर्क
एक प्राथमिक देखभाल नेटवर्क (पीसीएन) एक प्रकार का प्रदाता समूह है जो यूके में आम है। पीसीएन "सामान्य प्रथाओं के समूह हैं जो अपने रोगियों के लिए एकीकृत देखभाल प्रदान करने के लिए एक साथ काम करते हैं" (एनएचएस इंग्लैंड, 2020)।
एनएचएस फाउंडेशन ट्रस्ट
एनएचएस फाउंडेशन ट्रस्ट (एनएफटी) इंग्लैंड में एक प्रकार का प्रदाता है जो एनएचएस अस्पताल और या सामुदायिक स्वास्थ्य सेवाएं प्रदान करता है। एनएफटी "स्वायत्त, सार्वजनिक रूप से जवाबदेह संगठन" हैं जो "एनएचएस के भीतर काम करते हैं और दिन-प्रतिदिन के सरकारी नियंत्रण से मुक्त हैं" (एनएचएस फाउंडेशन ट्रस्ट, 2020)। एनएचएस फाउंडेशन ट्रस्ट अक्सर कई अस्पताल और सामुदायिक साइटों पर काम करते हैं।
अकादमिक स्वास्थ्य विज्ञान केंद्र
एक अकादमिक स्वास्थ्य विज्ञान केंद्र (एएचएससी) एक प्रकार का प्रदाता है जो अमेरिका, ब्रिटेन और कनाडा में आम है। एएचएससी "विश्वविद्यालय और शिक्षण अस्पताल हैं जो रोगी देखभाल की गुणवत्ता में सुधार, चिकित्सा शिक्षा और प्रशिक्षण को आगे बढ़ाने और ग्राउंडब्रैकिंग अनुसंधान करने के लिए सेना में शामिल हो गए हैं" (एसोसिएशन ऑफ अमेरिकन मेडिकल कॉलेज, 2020)।
सैन्य अस्पताल
ये अस्पताल हैं जो सेना द्वारा चलाए जाते हैं और वे सशस्त्र बलों के सदस्यों और उनके परिवारों की देखभाल करते हैं। सैन्य अस्पताल दुनिया भर के कई देशों में पाए जाते हैं।
प्रदाता समेकन की ओर रुझान
हाल के वर्षों में हेल्थकेयर सेक्टर में कंसॉलिडेशन का रुझान बढ़ा है। इसका मतलब है कि प्रदाता समूहों की बढ़ती संख्या और इन समूहों के आकार में वृद्धि हुई है। इस समेकन के कारण हैं:
- देखभाल की गुणवत्ता में सुधार करने के लिए
- लागत को कम करने के लिए
- दक्षता बढ़ाने के लिए
- देखभाल तक पहुंच में सुधार करने के लिए
समेकन की दिशा में रुझान भविष्य में जारी रहने की संभावना है क्योंकि प्रदाता समूह अपने पैमाने और दायरे को बढ़ाने के तरीकों की तलाश करते हैं।
प्रदाता संगठन और एकीकृत देखभाल
एकीकृत देखभाल प्रदान करने के लिए प्रदाताओं को एक साथ काम करने के लिए रणनीतिक खरीद के उपयोग की दिशा में बढ़ती प्रवृत्ति है। प्रदाताओं ने कैसे प्रतिक्रिया दी है, इसके उदाहरणों में जवाबदेह देखभाल संगठनों की स्थापना, एकीकृत वितरण नेटवर्क और प्राथमिक देखभाल चिकित्सकों के लिए अस्पताल प्रणालियों से जुड़े या संबद्ध होने की बढ़ती प्रवृत्ति शामिल है।
हेल्थकेयर परचेजिंग और हेल्थकेयर प्रोविजन के बीच एकीकरण की दिशा में भी रुझान है। यहाँ कुछ उदाहरण दिए गए हैं:
प्रबंधित देखभाल संगठन
एक प्रबंधित देखभाल संगठन (एमसीओ) एक प्रकार का प्रदाता समूह है जो नामांकित लोगों के एक समूह को स्वास्थ्य सेवाएं प्रदान करता है। अमेरिका में एमसीओ आम हैं और वे या तो लाभ के लिए या गैर-लाभकारी हो सकते हैं। उन्हें कभी-कभी इंटीग्रेटर्स के रूप में संदर्भित किया जाता है क्योंकि वे आमतौर पर देखभाल के वितरण के लिए बीमा निधि और सेवा प्रदाताओं के बीच इंटरफेस पर काम कर सकते हैं।
स्वास्थ्य रखरखाव संगठन
एक स्वास्थ्य रखरखाव संगठन (एचएमओ) एक विशिष्ट प्रकार का प्रबंधित देखभाल संगठन है। वे एक निश्चित मूल्य के लिए आबादी को देखभाल प्रदान करने के सिद्धांत पर काम करते हैं।
पहला एचएमओ संयुक्त राज्य अमेरिका में स्थापित किया गया था, 1929 में, रॉस-लूस मेडिकल ग्रुप। अंतर्राष्ट्रीय उदाहरणों में इज़राइल शामिल है जिसमें क्षेत्रीय रूप से आधारित एचएमओ हैं और सभी निवासियों को कम से कम एक के साथ पंजीकृत होना चाहिए। अन्य उदाहरणों में फिलीपींस और नाइजीरिया शामिल हैं।
एचएमओ के अलग-अलग ऑपरेटिंग मॉडल हैं; वे कर्मचारियों को नियुक्त कर सकते हैं और देखभाल प्रदान कर सकते हैं, देखभाल को सुरक्षित करने के लिए प्रदाताओं के नेटवर्क के साथ देखभाल या अनुबंध देने के लिए स्व-नियोजित या स्वास्थ्य पेशेवरों के समूहों के साथ अनुबंध कर सकते हैं।
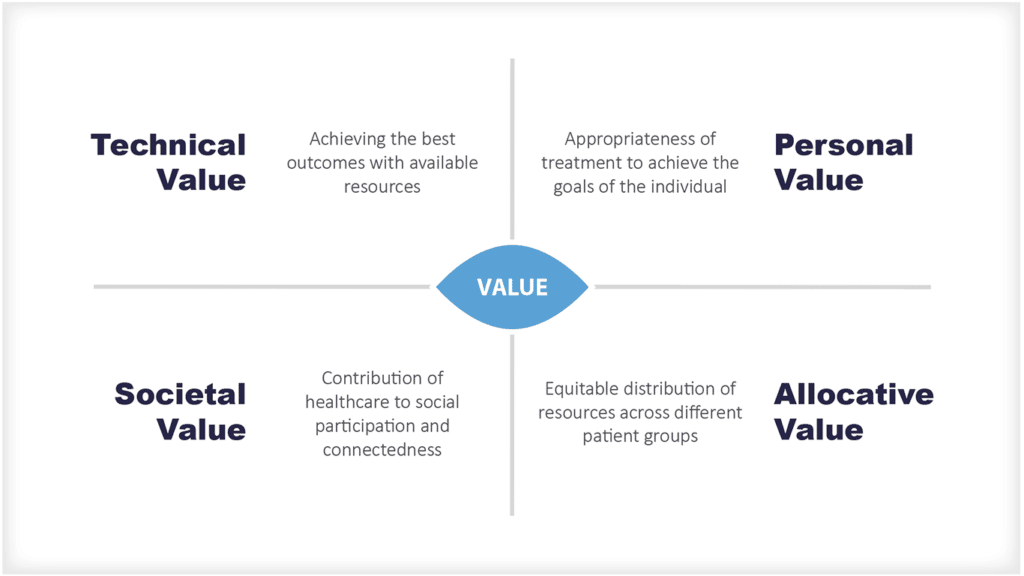
स्वास्थ्य देखभाल प्रदाता आर्थिक मूल्य में सुधार कैसे कर सकते हैं?
स्वास्थ्य सेवाओं की डिलीवरी एक स्वास्थ्य सेवा प्रणाली का मुख्य कार्य है। इसलिए, स्वास्थ्य सेवा प्रदाताओं को यह सुनिश्चित करने में एक बड़ी भूमिका निभानी है कि संसाधनों का प्रभावी ढंग से और कुशलता से उपयोग किया जाता है और मूल्य प्रदान किया जाता है:
- गुणवत्ता में सुधार और स्वास्थ्य देखभाल परिणामों में सुधार करके
- सुरक्षित रूप से सेवाएं प्रदान करके और यह सुनिश्चित करके कि रोगियों को सही समय पर सही उपचार प्राप्त हो और संक्रमण जैसे स्वास्थ्य जोखिमों के संपर्क में न आएं
- लागत को नियंत्रित करके
- संसाधनों के उपयोग में उत्पादकता और दक्षता में वृद्धि करके
- स्वास्थ्य सेवा तक पहुंच में सुधार करके
रणनीतिक क्रय और प्रदाता भुगतान मॉडल प्रदाताओं को मूल्य बढ़ाने के लिए समर्थन और प्रोत्साहित कर सकते हैं, जैसे कि सिस्टम पूरी तरह से मूल्य-आधारित देखभाल प्रदान कर सकता है।
उपयोगी संदर्भ
अमेरिकन मेडिकल कॉलेजों का संघ। (2020). अकादमिक स्वास्थ्य विज्ञान केंद्र।
एनएचएस इंग्लैंड। एकीकृत देखभाल साझेदारी: एसटीपी और आईसीएस के लिए अवलोकन और मार्गदर्शन।
रॉस, जेएम, और लूस, डब्ल्यूएच (1929)। एक नए प्रकार की चिकित्सा पद्धति: अस्पताल के बिना समूह अभ्यास। न्यू इंग्लैंड जर्नल ऑफ मेडिसिन, 201 (17), 788-793।
अमेरिकी स्वास्थ्य और मानव सेवा विभाग। (एन.डी.)। एक एचएमओ क्या है?
वोल्टर्स क्लूवर। स्वास्थ्य सेवा उद्योग में समेकन: ड्राइवर, लाभ और चुनौतियां।