Introducción a los objetivos del sistema sanitario
Las metas del sistema sanitario son los objetivos que un sistema sanitario se fija para mejorar la salud de la población y el rendimiento del sistema sanitario. Estos objetivos pueden establecerse a diferentes niveles, desde el mundial hasta el nacional y el local.
Los objetivos de resultados sanitarios globales, establecidos por las Naciones Unidas, incluyen, por ejemplo
- reducir la mortalidad materna
- reducir las muertes evitables de niños menores de 5 años
- reducir el riesgo de enfermedades transmisibles
- reducir las muertes y lesiones por accidentes de tráfico
Sin embargo, no existe un consenso internacional sobre la mejor manera de medir el rendimiento del sistema sanitario.
El contexto de cada país es importante y el estado actual de la salud de la población y de la madurez del sistema sanitario tiene una enorme repercusión en los objetivos que pueden fijarse y en los que pueden alcanzarse.
A nivel nacional, los objetivos del sistema sanitario varían en función de las necesidades específicas de un país. Sin embargo, algunos de los objetivos comunes que pueden establecerse a este nivel son la mejora del acceso a la asistencia sanitaria, el aumento de la calidad de la atención y la reducción de los costes sanitarios.
Los objetivos del sistema sanitario local también variarán en función de las necesidades de una comunidad o población concreta. Sin embargo, algunos objetivos comunes que podrían establecerse a este nivel incluyen el aumento del número de personas que reciben atención preventiva, la reducción de las disparidades sanitarias y la mejora de la coordinación de la atención.
Este artículo explora los diferentes tipos de objetivos de los sistemas sanitarios y cómo se miden.
Qué son los 13 Objetivos Sanitarios Mundiales
En 2015, las Naciones Unidas establecieron 17 objetivos de desarrollo sostenible para 2030, muchos de los cuales afectan a la salud y el bienestar.
El Objetivo de Desarrollo Sostenible 3 (ODS 3) es
"garantizar una vida sana y promover el bienestar para todos en todas las edades".
Hay 13 objetivos:
- Para 2030, reducir la tasa de mortalidad materna mundial a menos de 70 por cada 100.000 nacidos vivos
2.Para 2030, poner fin a las muertes evitables de recién nacidos y de niños menores de 5 años, con el objetivo de que todos los países reduzcan la mortalidad neonatal a un mínimo de 12 por cada 1.000 nacidos vivos y la mortalidad de menores de 5 años a un mínimo de 25 por cada 1.000 nacidos vivos.
- Para 2030, poner fin a las epidemias de sida, tuberculosis, paludismo y enfermedades tropicales desatendidas y combatir la hepatitis, las enfermedades transmitidas por el agua y otras enfermedades transmisibles
- Para 2030, reducir en un tercio la mortalidad prematura por enfermedades no transmisibles mediante la prevención y el tratamiento y promover la salud mental y el bienestar
- Para 2030, reforzar la prevención y el tratamiento del abuso de sustancias, incluido el abuso de estupefacientes y el uso nocivo del alcohol.
- Para 2030, reducir a la mitad el número de muertos y heridos por accidentes de tráfico en el mundo
- Para 2030, garantizar el acceso universal a los servicios de atención a la salud sexual y reproductiva, incluidos los de planificación familiar, información y educación, y la integración de la salud reproductiva en las estrategias y programas nacionales.
- Lograr la cobertura sanitaria universal, incluida la protección contra riesgos financieros, el acceso a servicios sanitarios esenciales de calidad y el acceso a medicamentos y vacunas esenciales seguros, eficaces, de calidad y asequibles para todos.
- Para 2030, reducir sustancialmente el número de muertes y enfermedades debidas a productos químicos peligrosos y a la contaminación del aire, el agua y el suelo.
- Para 2030, reducir sustancialmente el número de muertes y enfermedades debidas a productos químicos peligrosos y a la contaminación del aire, el agua y el suelo
- Reforzar la aplicación del Convenio Marco de la Organización Mundial de la Salud para el Control del Tabaco en todos los países, según proceda
- Apoyar la investigación y el desarrollo de vacunas y medicamentos para las enfermedades transmisibles y no transmisibles que afectan principalmente a los países en desarrollo, proporcionar acceso a medicamentos y vacunas esenciales asequibles, de conformidad con la Declaración de Doha sobre el Acuerdo ADPIC y la Salud Pública, que afirma el derecho de los países en desarrollo a utilizar plenamente las disposiciones del Acuerdo sobre los Aspectos de los Derechos de Propiedad Intelectual relacionados con el Comercio en relación con las flexibilidades para proteger la salud pública y, en particular, proporcionar acceso a los medicamentos para todos.
- Reforzar la capacidad de todos los países, en particular de los países en desarrollo, para la alerta temprana, la reducción de riesgos y la gestión de los riesgos sanitarios nacionales y mundiales.
Hay muchas más metas relacionadas con la salud en los Objetivos de Desarrollo Sostenible, como la mejora de la dieta y la seguridad alimentaria, el acceso a la educación, el acceso al agua potable, etc.
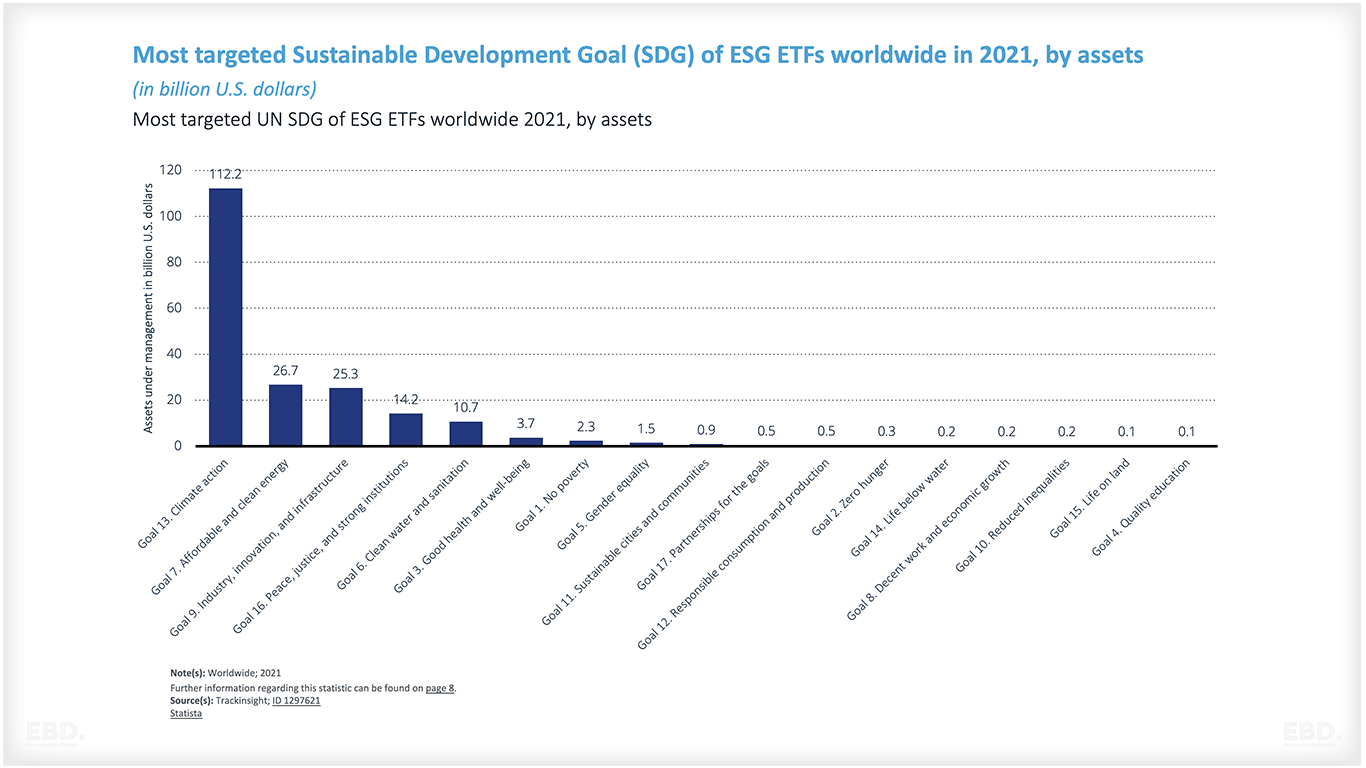
El ODS 3 ocupa el sexto lugar de los 17 ODS en cuanto a la inversión en Fondos de Intercambio Ambiental, Social y de Gobernanza (ETF) en 2021 a nivel mundial.
El Plan de Acción Mundial para Vidas Saludables y Bienestar para Todos (SGD3 GAP) cuenta con la participación de 13 socios y organismos mundiales y se creó para apoyar a los gobiernos en la consecución de los Objetivos de Desarrollo Sostenible relacionados con la salud.
¿Cuáles son algunos de los objetivos comunes del sistema sanitario nacional?
Hay una variedad de tipos de objetivos que los sistemas sanitarios pueden establecer a diferentes niveles. Algunos ejemplos de objetivos del sistema sanitario son:
- Mejorar el acceso a la asistencia sanitaria: Puede tratarse de aumentar el número de proveedores de atención primaria en una comunidad o de garantizar que todos los residentes tengan un seguro médico.
- Mejorar la calidad de la atención: Esto podría implicar el aumento de la seguridad del paciente o garantizar que todos los pacientes reciban una atención basada en la evidencia.
- Reducir los costes sanitarios: Esto podría implicar la reducción de pruebas y procedimientos innecesarios o la mejora de la eficiencia del sistema sanitario.
- Reducir las disparidades sanitarias: Esto podría implicar el aumento del número de residentes de minorías que reciben atención preventiva o la prestación de atención culturalmente competente a todos los pacientes.
- Mejorar la coordinación de la atención: Esto podría implicar aumentar el número de pacientes que ven a un proveedor de atención primaria de forma regular o garantizar que todos los pacientes tengan un hogar médico.
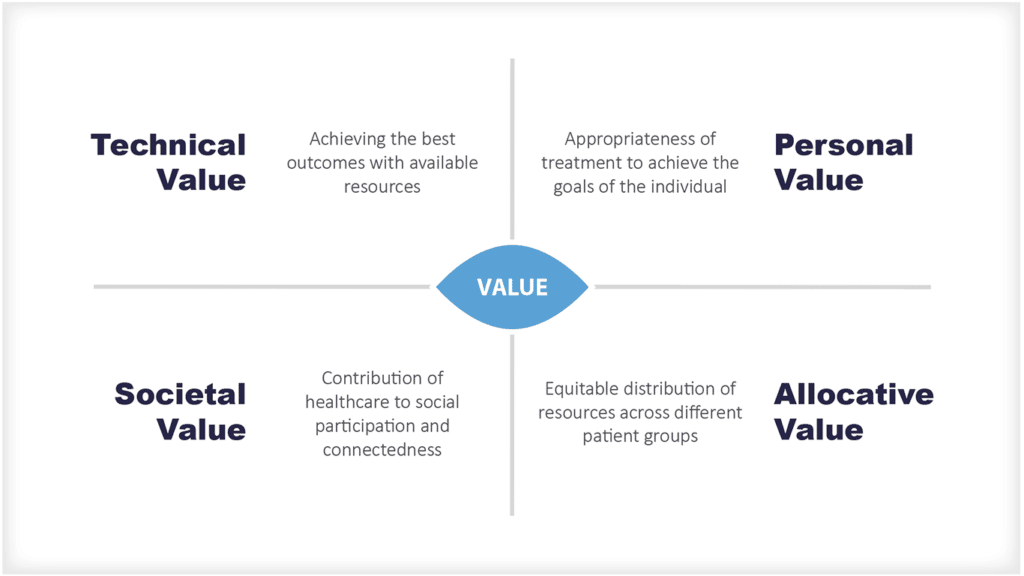
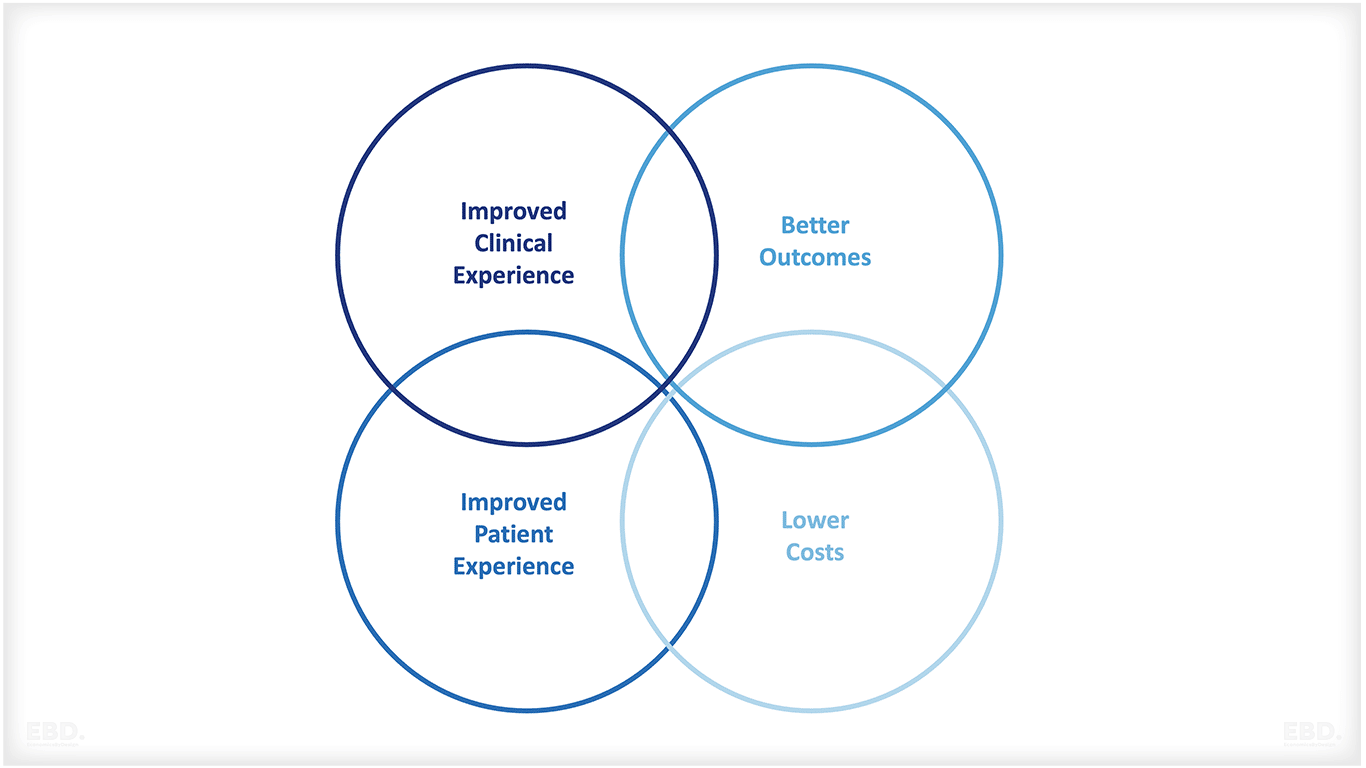
Los sistemas sanitarios utilizan cada vez más marcos de atención sanitaria basados en el valor, como el triple objetivo o el cuádruple objetivo, para enmarcar los objetivos de los sistemas sanitarios nacionales.
Resultados sanitarios
La Organización Mundial de la Salud (OMS) define los resultados sanitarios como "el estado de salud de una persona o población en un momento determinado o a lo largo de un periodo de tiempo, que puede medirse mediante diversos indicadores". En otras palabras, los resultados sanitarios son el resultado final del estado de salud de una persona o población.
Hay muchos tipos diferentes de resultados sanitarios, pero pueden clasificarse a grandes rasgos en dos categorías principales: resultados de mortalidad y resultados de morbilidad.
Resultados de la mortalidad
Se refieren al número de muertes que se producen en una población durante un periodo determinado. Estos resultados pueden subdividirse en mortalidad por todas las causas (el número total de muertes por todas las causas) y mortalidad por causas específicas (el número de muertes por una causa específica).
Resultados de la morbilidad
Se refieren al número de personas de una población que experimentan una determinada condición de salud o enfermedad durante un período específico. La morbilidad puede medirse en términos de prevalencia (el número de personas con una afección en un momento dado) o de incidencia (el número de nuevos casos de una afección en un periodo de tiempo determinado).
Los resultados sanitarios son importantes porque proporcionan una medida de si la salud de una población está mejorando, empeorando o permaneciendo estable a lo largo del tiempo. También permiten hacer comparaciones entre diferentes poblaciones (por ejemplo, entre diferentes países o regiones) y pueden ayudar a identificar áreas en las que es necesario intervenir para mejorar la salud de una población.
Son muchos los factores que pueden influir en los resultados sanitarios. Estos incluyen, pero no se limitan a:
- La calidad de la asistencia sanitaria: Incluye factores como la disponibilidad de atención preventiva y tratamiento, la eficacia de la atención y la seguridad del paciente.
- Situación socioeconómica: Se refiere a factores como los ingresos, la educación y el empleo. Está bien establecido que las personas con un estatus socioeconómico más bajo tienen más probabilidades de experimentar peores resultados de salud.
- Los determinantes sociales de la salud: Son las condiciones en las que la gente vive, trabaja y juega. Incluyen factores como la vivienda, el transporte y el acceso a alimentos saludables. Los determinantes sociales de la salud tienen un impacto significativo en los resultados sanitarios.
- Factores de riesgo para la salud: Son los comportamientos y condiciones que aumentan la probabilidad de desarrollar una enfermedad o experimentar un evento de salud adverso. Ejemplos comunes de factores de riesgo para la salud son el tabaquismo, la obesidad y la hipertensión arterial.
La lista anterior no es en absoluto exhaustiva, pero ofrece una visión general de algunos de los principales factores que pueden influir en los resultados sanitarios.
¿Cuáles son algunos de los retos asociados al establecimiento de objetivos del sistema sanitario?
El establecimiento de los objetivos del sistema sanitario plantea numerosos retos. Estos retos incluyen, entre otros, los siguientes:
Coste
Muchas intervenciones sanitarias pueden ser costosas, y puede ser difícil encontrar los recursos para aplicarlas a gran escala.
Viabilidad
Algunas intervenciones sanitarias podrían no ser factibles de aplicar en un entorno determinado. Por ejemplo, una intervención que requiere un alto nivel de recursos podría no ser factible de aplicar en un entorno con pocos recursos.
Sostenibilidad
Puede ser difícil mantener las intervenciones sanitarias a largo plazo. Esto suele deberse a factores como los cambios en la financiación o la dotación de personal.
Evaluación
Puede ser difícil evaluar el impacto de las intervenciones sanitarias, sobre todo cuando hay múltiples factores que pueden influir en los resultados sanitarios.
Voluntad política
Es necesario que haya suficiente voluntad política para aplicar las intervenciones sanitarias a gran escala. Esto puede ser difícil de conseguir, sobre todo cuando hay prioridades que compiten entre sí.
A pesar de estos retos, es importante establecer objetivos para el sistema sanitario con el fin de mejorar la salud de la población. El establecimiento de objetivos puede ayudar a centrar la atención y los recursos en los problemas de salud prioritarios, y puede proporcionar un marco para evaluar el impacto de las intervenciones sanitarias.
¿Cuáles son algunos consejos para fijar los objetivos del sistema sanitario?
Hay una serie de cosas que hay que tener en cuenta a la hora de fijar los objetivos del sistema sanitario. Estos consejos pueden ayudar a garantizar que los objetivos sean realistas y alcanzables:
Consultar con las partes interesadas
Es importante consultar con las principales partes interesadas a la hora de establecer los objetivos del sistema sanitario. Esto ayudará a garantizar que los objetivos estén alineados con las necesidades de la población.
Establezca objetivos realistas
Es importante establecer objetivos realistas que puedan alcanzarse en un plazo razonable. Establecer objetivos poco realistas puede llevar a la frustración y a la desilusión.
Sea específico
Los objetivos deben ser específicos para poder ser medibles. Por ejemplo, en lugar de establecer un objetivo de "mejorar el acceso a la atención sanitaria", un objetivo más específico podría ser "aumentar el número de proveedores de atención primaria en una comunidad".
Utilizar los datos existentes
A la hora de establecer los objetivos del sistema sanitario, utilice las fuentes de datos existentes, como las encuestas nacionales de salud. Esto ayudará a garantizar que los objetivos se basen en pruebas.
Busque la opinión de los expertos
A la hora de establecer los objetivos del sistema sanitario, solicite la opinión de expertos en la materia. Esto ayudará a garantizar que los objetivos sean alcanzables y realistas.
¿Cuáles son algunos ejemplos de objetivos del sistema sanitario?
Hay una serie de posibles objetivos del sistema sanitario que podrían establecerse. Estos objetivos pueden centrarse en la mejora de la calidad de la atención, la reducción de los costes sanitarios o la reducción de las disparidades sanitarias. Algunos ejemplos de objetivos del sistema sanitario son:
- Aumentar el número de proveedores de atención primaria en una comunidad.
- Garantizar que todos los pacientes reciban una atención basada en la evidencia.
- Reducir las pruebas y procedimientos innecesarios.
- Mejorar la eficiencia del sistema sanitario.
- Aumentar el porcentaje de pacientes que reciben atención preventiva.
- Reducir las disparidades sanitarias entre los distintos grupos de población.
- Mejorar la calidad de la atención a las enfermedades crónicas.
- Reducción de la tasa de reingresos hospitalarios.
- Aumentar la satisfacción de los pacientes con el sistema sanitario.
- Mejora de los resultados sanitarios de la población.
Es importante establecer objetivos para el sistema sanitario que estén basados en la evidencia y sean alcanzables. Sin embargo, también es importante ser consciente de los retos que pueden estar asociados a la fijación de objetivos. Estos retos incluyen la viabilidad, la rentabilidad y la equidad.
Atención sanitaria basada en el valor y resultados sanitarios
La asistencia sanitaria basada en el valor es un enfoque de la asistencia sanitaria que se centra en mejorar los resultados de los pacientes. Esto significa que, en lugar de centrarse simplemente en la prestación de asistencia, la asistencia sanitaria basada en el valor también tiene en cuenta los resultados de salud de los pacientes.
Un ejemplo de objetivo sanitario basado en el valor podría ser la reducción del número de reingresos hospitalarios. Este objetivo se centraría en mejorar los resultados de los pacientes garantizando que no se les dé el alta demasiado pronto y que luego tengan que ser readmitidos.
Otro ejemplo podría ser mejorar los resultados sanitarios de la población a nivel de los ciudadanos. Esto podría implicar el establecimiento de objetivos como la reducción de las tasas de tabaquismo o el aumento de las tasas de vacunación.
La consecución de este tipo de objetivos puede requerir un enfoque multisectorial, así como centrarse en la promoción de la salud y la prevención de enfermedades. Es importante recordar que este tipo de objetivos requiere un compromiso a largo plazo y no puede lograrse de la noche a la mañana.
Al establecer los objetivos del sistema sanitario, es importante tener en cuenta las necesidades de todas las partes interesadas. Esto incluye a los pacientes, los proveedores, los pagadores y la comunidad. Los objetivos deben ser alcanzables y realistas, y deben basarse en la evidencia.
Atención centrada en el paciente
La atención centrada en el paciente es un enfoque de la asistencia sanitaria que se centra en satisfacer las necesidades del paciente. Esto significa que, en lugar de limitarse a prestar atención, la atención centrada en el paciente también tiene en cuenta sus preferencias y valores.
Un ejemplo de objetivo centrado en el paciente podría ser garantizar que todos los pacientes tengan acceso a su historial médico. Esto permitiría a los pacientes participar más en su propia asistencia sanitaria y tomar decisiones informadas sobre su tratamiento.
Otro ejemplo podría ser mejorar la comunicación entre pacientes y proveedores. Esto podría implicar el establecimiento de objetivos como el aumento del número de visitas entre el proveedor y el paciente que se realizan cara a cara, o garantizar que todas las llamadas telefónicas y los correos electrónicos se devuelven en un plazo de 24 horas.
La consecución de este tipo de objetivos puede exigir un cambio en la forma de prestar la asistencia sanitaria. Es importante recordar que este tipo de objetivos requiere un compromiso a largo plazo y no puede lograrse de la noche a la mañana.
Al establecer los objetivos del sistema sanitario, es importante tener en cuenta las necesidades de todas las partes interesadas. Esto incluye a los pacientes, los proveedores, los pagadores y la comunidad. Los objetivos deben ser alcanzables y realistas, y deben basarse en la evidencia.
¿Qué son las métricas de resultados comunicadas por los pacientes?
Las métricas de resultados comunicados por los pacientes (PROM) son un tipo de métrica centrada en el paciente que se centra en los resultados que son importantes para los pacientes. Esto significa que, en lugar de limitarse a medir la prestación de la atención, las PROM también tienen en cuenta los resultados de salud de los pacientes.
Un ejemplo podría ser medir el número de pacientes que experimentan una complicación de salud tras el alta hospitalaria. Esto podría ayudar a identificar posibles problemas con la atención que reciben los pacientes y asegurarse de que reciben la mejor atención posible.
¿Qué son las métricas de la experiencia reportada por los pacientes?
Las métricas de la experiencia del paciente (PREM) son un tipo de métrica centrada en el paciente que se centra en las experiencias de los pacientes. Esto significa que, en lugar de limitarse a medir la prestación de la atención, las PREM también tienen en cuenta la forma en que los pacientes se sienten con respecto a su atención.
Un ejemplo podría ser medir el número de pacientes que están satisfechos con la atención recibida. Esto podría ayudar a identificar las áreas en las que los pacientes no están satisfechos con su atención y asegurarse de que están recibiendo la mejor atención posible.
¿Cuál es la diferencia entre un objetivo y un indicador clave de rendimiento?
Un objetivo es un resultado deseado que las organizaciones sanitarias esperan alcanzar. Los indicadores clave de rendimiento (KPI) son un tipo de métrica que se utiliza para medir el progreso hacia un objetivo. Esto significa que los KPI pueden utilizarse para comprobar si una organización sanitaria avanza o no hacia sus objetivos.
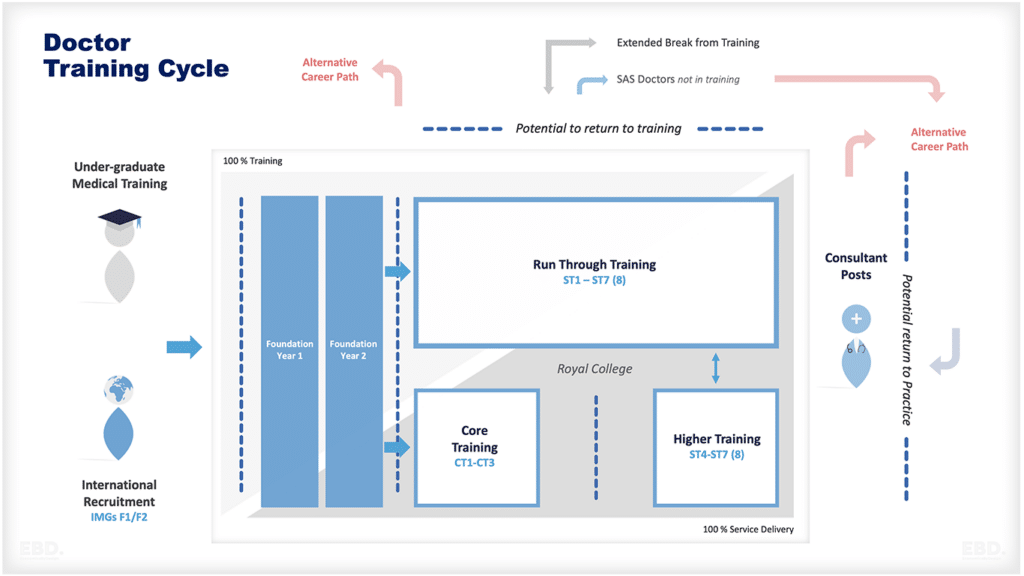
Objetivos del sistema sanitario en Inglaterra: Un estudio de caso
El Departamento de Salud y Asistencia Social (DHSC) es responsable de establecer la política del sistema sanitario en Inglaterra. Sus prioridades actuales son:
- proteger la salud pública mediante la respuesta del sistema sanitario y social a la COVID-19
- mejorar los resultados de la asistencia sanitaria proporcionando una atención de alta calidad y sostenible en el momento y lugar adecuados, así como mejorando las infraestructuras y transformando la tecnología
- mejorar los resultados de la atención sanitaria gracias a una plantilla bien respaldada
- mejorar, proteger y nivelar la salud de la nación, incluso reduciendo las disparidades sanitarias
- mejorar los resultados de la asistencia social mediante un sistema de asistencia social para adultos asequible, de alta calidad y sostenible
El último plan, publicado en septiembre de 2022, incluía los siguientes objetivos
- Garantizar el acceso a la atención primaria, con tiempos de espera de las citas iguales o inferiores a dos semanas.
- ayudar a las personas a pasar del hospital a la asistencia social cuando la necesiten
- apoyar a los médicos para que amplíen su carrera y mejorar el uso de voluntarios para apoyar los servicios sanitarios
NHS England es un organismo público ejecutivo no departamental responsable del NHS en Inglaterra. Depende del DHSC. El DHSC proporciona un mandato para que NHS England cumpla con las prioridades nacionales.
Para 2022-23, los 5 objetivos fijados por el DHSC para el NHS England eran los siguientes
- seguir liderando el NHS en la gestión del impacto del COVID-19 en la salud y la asistencia
- recuperar y mantener la prestación de servicios y funciones más amplias del NHS
- renovar el enfoque para cumplir con el plan a largo plazo del NHS y los compromisos más amplios para el NHS
- integrar un enfoque de gestión de la salud de la población en los sistemas locales, intensificando la acción para prevenir la mala salud y abordar las desigualdades sanitarias
- garantizar un liderazgo, una cultura y un uso de los recursos organizativos eficaces del NHS para obtener los beneficios de los futuros cambios estructurales en el ámbito sanitario y asistencial
A continuación, NHS England establece objetivos y metas para el NHS en Inglaterra. Éstos se establecen como guía de planificación operativa. Para 2022-23, estos se centraron en:
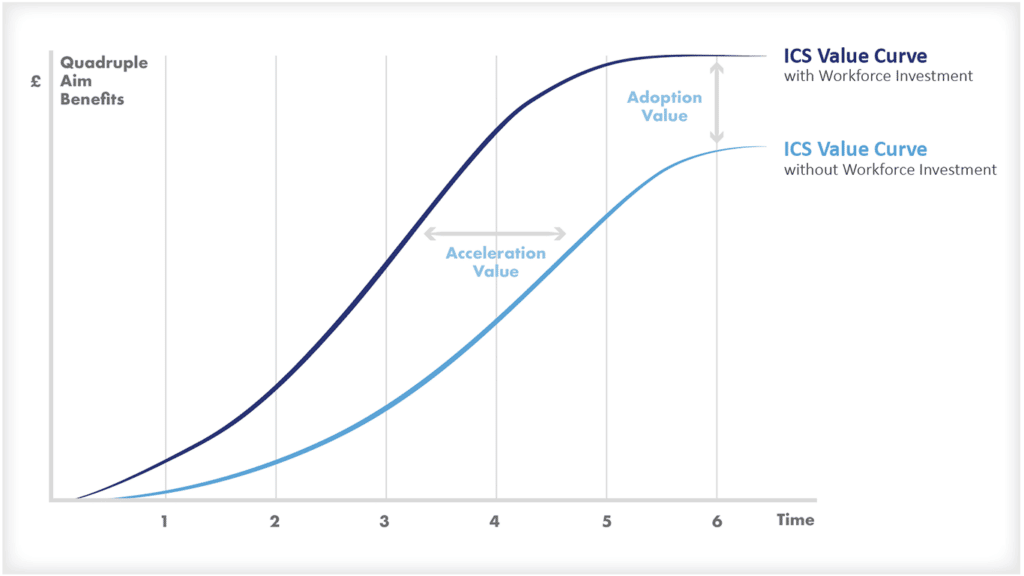
- inversión en mano de obra
- incluso más mejoras en la respuesta a Covid-19, incluyendo la vacunación y centrándose en el síndrome COVID-19 (long-covid)
- aumentar la prestación de atención electiva o planificada hasta el 110% de los niveles anteriores a la pandemia, a fin de resolver los atrasos y reducir los largos tiempos de espera, y abordar los desafíos particulares en relación con el cáncer, el diagnóstico y la atención a la maternidad
- mejorar la capacidad de respuesta de la atención de urgencia y emergencia, incluyendo la mejora de los servicios en la comunidad para permitir que se preste más atención en el hogar
- mejorar el acceso a la atención primaria
- mejorar los servicios de salud mental y para las personas con problemas de aprendizaje
- seguir desarrollando enfoques de gestión sanitaria de la población para mejorar la salud y reducir las desigualdades sanitarias
- lograr un nivel básico de digitalización en todos los servicios
- volver a los niveles de productividad anteriores a la pandemia
- el establecimiento de los 42 sistemas de atención integrada a partir de julio de 2022.
Los Sistemas de Atención Integrada tienen 4 objetivos generales:
- Mejorar los resultados de la salud y la asistencia sanitaria de la población
- Abordar las desigualdades en los resultados, la experiencia y el acceso
- Aumentar la productividad y la rentabilidad
- Ayudar al SNS a apoyar un desarrollo social y económico más amplio
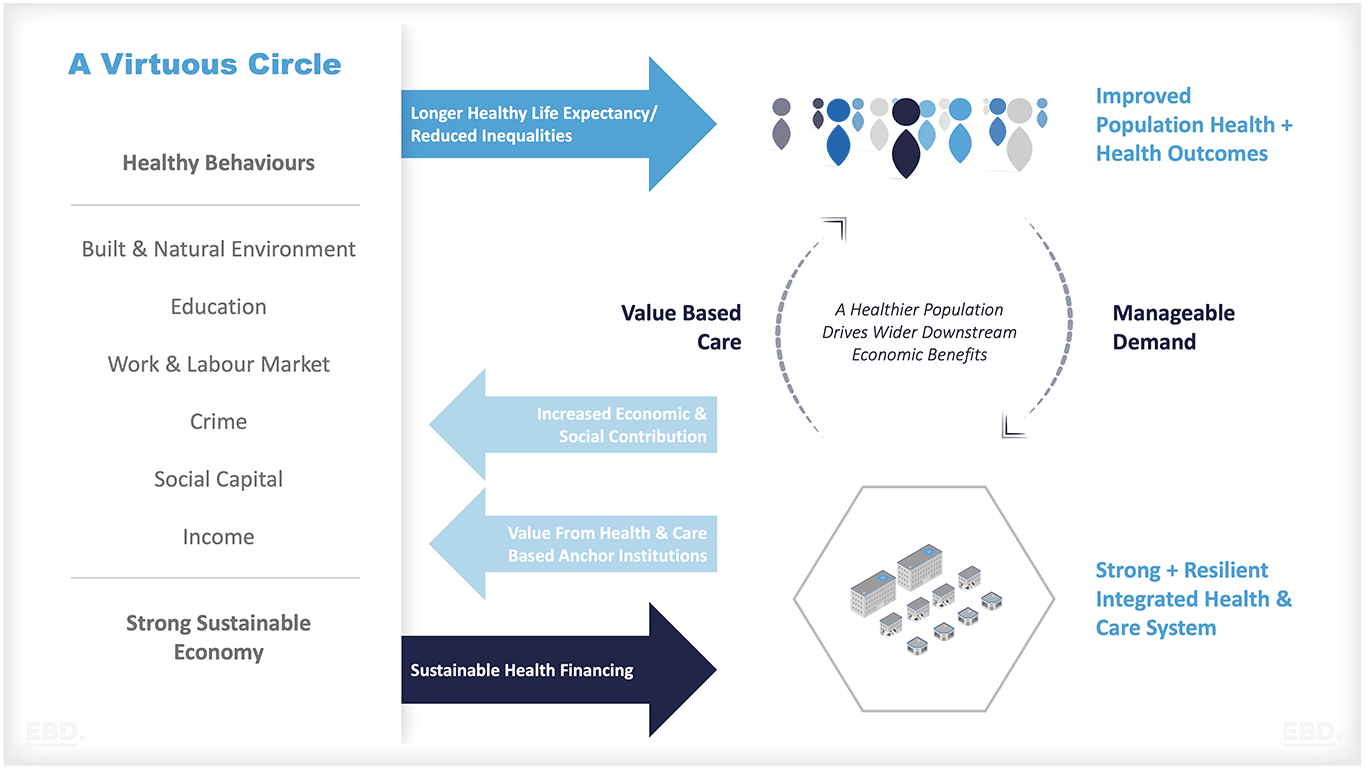
Cada Sistema Asistencial Integrado colaborará en el establecimiento de objetivos y metas locales para las zonas geográficas y organizaciones dentro del ámbito de su gobernanza. Esto incluirá metas y objetivos compartidos para el "lugar" y dentro de estos "barrios". Incluirá objetivos de salud pública, prestación de servicios sanitarios y asistencia social.
En el noroeste de Londres, por ejemplo, se han fijado objetivos de alto nivel para:
- identificar y abordar las desigualdades en el acceso, la experiencia y los resultados
- poner en marcha los elementos básicos de un enfoque sanitario de la población
- mejorar la salud y prevenir la enfermedad, tal y como se identifica en Core20PLUS5
- mejorar los factores sociales, ambientales y de vida saludable que afectan negativamente a la salud y el bienestar
Estos objetivos se transmitirán a la organización responsable respectiva (la Autoridad Local y la Junta de Atención Integrada) y a los proveedores a través de la compra y la contratación estratégicas.
NHS England ha establecido 8 objetivos para los sistemas de atención integrada para el invierno de 2022:
- Prepararse para las variantes de COVID-19 y los desafíos respiratorios, incluyendo un programa integrado de vacunación contra el COVID-19 y la gripe.
- Aumentar la capacidad fuera de los centros de agudos, incluyendo la ampliación de funciones adicionales en atención primaria y la liberación de fondos anuales para apoyar la salud mental durante el invierno.
- Aumentar la resistencia de los servicios 111 y 999 del NHS, mediante el incremento del número de gestores de llamadas hasta 4,8k en el 111 y 2,5k en el 999.
- Objetivo de los tiempos de respuesta de la categoría 2 y de los retrasos en el traspaso de las ambulancias, incluida la mejora de la utilización de los servicios de respuesta comunitaria urgente y de respuesta rápida, la nueva plataforma digital de enrutamiento inteligente y el apoyo directo a los fideicomisos con más dificultades.
- Reducir las aglomeraciones en los servicios de urgencias y centrarse en las esperas más prolongadas en los servicios de urgencias, mejorando el uso del directorio de servicios del NHS y aumentando la provisión de atención de urgencias en el mismo día y de servicios para personas frágiles.
- Reducir la ocupación hospitalaria, aumentando la capacidad en el equivalente de al menos 7.000 camas generales y de agudos, mediante una combinación de nuevas camas físicas, salas virtuales y mejoras en otros puntos de la vía.
- Garantizar el alta oportuna, en los entornos de agudos, salud mental y comunidad, trabajando con los socios de atención social y aplicando las 10 intervenciones de mejores prácticas a través del "reto de los 100 días".
- Proporcionar un mejor apoyo a las personas en casa, incluyendo la ampliación de las salas virtuales y el apoyo adicional a los usuarios de alta intensidad con necesidades complejas.
El seguimiento se realizará a través de 6 métricas:
- Abandono de llamadas al 111. (El 111 es un sistema de triaje telefónico para la atención urgente)
- Tiempos medios de respuesta de las llamadas al 999. (El 999 es un sistema de triaje telefónico para los servicios de emergencia, incluidos los servicios de ambulancia)
- Tiempos de respuesta de las ambulancias de categoría 2. (la categoría 2 es una emergencia o una afección grave que puede requerir una evaluación rápida, una intervención en el lugar de los hechos o un transporte urgente al hospital)
- Promedio de horas perdidas por día por retrasos en el traspaso de ambulancias.
- Ocupación de camas generales y de agudos de tipo 1 para adultos (ajustada por las camas vacías). (fideicomisos de agudos con departamentos de emergencias mayores)
- Porcentaje de camas ocupadas por pacientes que ya no cumplen los criterios de residencia.